Podoconiosis: A guide for farmers
Pennie Mills BSc (Hons) Podiatry
Jun
21
Jun
21
The study explores the experience and views of occupational therapists in stroke rehabilitation regarding knowledge translation. The apparent knowledge translation gap is described as the delay of use of research evidence into clinical practice.
A qualitative, descriptive research design was used. The verbatim transcripts of the interviews with special section neurology practice (SSNP) occupational therapists were coded and analyzed using thematic analysis.
The themes identified included 1) how occupational therapists responded to change, 2) how knowledge translation barriers could be seen as learning needs and may lead to empowerment, 3) the use of knowledge translation strategies and professional body support.
Knowledge translation barriers need to be identified in each single environment in order to recommend solutions. To improve knowledge translation training is needed in time management, coping strategies, assistance through supervision and managerial involvement to prevent workplace burn out. Personal initiatives must become natural, and networking similar to ‘communities of practice’ may keep healthcare professionals ahead of change. Learning needs appear to exist for clinicians and researchers., and improving knowledge translation in the future lies in personal initiative, innovation and involvement.
Graham (2006) highlighted that new developments in health research are often a delayed and the process is uncoordinated, resulting in patients not receiving the optimum interventions due to the late transfer of new knowledge into practice. The definition of knowledge translation (KT) by the World Health Organization (WHO, 2005) is “the synthesis, exchange and application of knowledge by relevant stakeholders to accelerate the benefits of global and local innovation in strengthening health systems and improving people’s health”. Knowledge translation in other words is the bridge between discovery and impact of evidence (Tetroe, 2008) and, as it has developed, it has been adopted by nursing, medicine and public health. The word knowledge used in the KT context means primarily scientific research (Graham, 2006).
“Evidence-based practice (EBP) is essentially a clinical decision making framework that encourages clinicians to integrate information from high quality quantitative and qualitative research with the clinician’s clinical expertise and the client’s background, preferences and values when making decisions” (Sackett et al. 1996, p. 71). Evidence-Based Practice (EBP) is seen as an essential part of the day to day work of occupational therapists (OT) and other health professionals.
The results from a multidisciplinary team study by Humphries et al. (2000) suggested that occupational therapists want to base their practice on research outcomes but find the ever-growing amount of evidence difficult to manage. Additionally, they highlighted time restrictions, workload pressures and staff shortages as barriers to evidence-based practice. Over a decade later similar factors remain on the list of barriers (Menon et al., 2010; McCluskey et al., 2013). Therefore, for EBP to work the theory-practice gap has to be bridged by developing KT strategies (Graham, 2006).
KT has developed immensely over the last twenty years (Grimshaw et al., 2012) to translate evidence into practice. Kielhofner (2005) explored the vast field of stakeholders involved in KT and suggested that more cooperation and teamwork between researchers and clinicians would facilitate more effective KT. Bayley et al. (2012) recommended that guideline developers set priorities in the way they transfer evidence into guidelines and employ easy to use language.
Jansen et al. (2012) performed a cross-sectional survey using focus groups and a two-round Delphi process to explore barriers to KT. The sample included 166 clinicians with varying academic degrees and professional backgrounds. Lack of time, access and the skills to use and appraise evidence-based literature were cited as barriers for clinicians not being up to date with the latest research. Although there was a low response rate of 38%, results highlighted that the allied health professionals (AHP) which included over 10 disciplines (occupational therapists, physiotherapists, dieticians, social workers and speech pathologists) used their colleagues and own experience as their most frequent evidence base, a finding supported by McKenna et al (2005) with occupational therapists. While physiotherapists had more positive results due to having adequate equipment, the occupational therapists reported missing relevance to practice in articles and lacking equipment at workplace to implement research into practice.
McCluskey and Middleton (2010) with community rehabilitation teams, Wilkinson (2012) with allied health staff, and Hughes et al. (2014) with healthcare professionals demonstrated that EBP had not been fully put into practice by the allied health professions. Solutions were identified as a need to change the behaviour of the allied health professions, more training in EBP and involvement in research, but also support from management. In summary, these studies have highlighted that similar barriers to KT still exist in contemporary practice. Suggestions to improve KT have included using peer support networks to promote EBP, and more equipment and training to improve access to research and in appraising information on the web.
The Health and Care Professionals Council (HCPC) requires health professions to maintain standards of proficiency and conduct which include the use of evidence-based practice in order “to be able to draw on appropriate knowledge and skills to inform practice” (HCPC, 2014, p. 12). Clinical guidelines are developed based on research evidence to advise health professionals in their practice. Some guidelines such as the National Clinical Guidelines for Stroke (NCGS) and the International Classifications of Functioning, Disability and Health (ICF) were developed to guide practice of healthcare professions working in neurorehabilitation settings. Hammond et al. (2005) utilized a retrospective audit to determine whether occupational therapists and physiotherapists showed complete compliance with the NCGS and found that there was surprisingly low adherence to them with more than 40% of admitted patients not seen within the recommended time frame, although the reasons for this lack of implementation were not explored. Wiseman-Hakes et al. (2012) highlighted the importance of considering context in EBP and KT and suggested a wider perspective in the definition of EBP. In a suggested list of ‘key questions’ for EBP they asked for the reasons why recommended interventions worked in a study, under which conditions they worked, for which clients and at what point of their progress they were applicable? The answers to the key questions could provide better information to clinicians and thereby support correct and easier implementation. In summary, although health research evidence is part of policy and guidelines, health professionals still utilize other factors as part of the clinical reasoning process to discern the relevance of this evidence, for example, empirical knowledge and individual patient context, including their preferences, vulnerabilities and co morbidities (Benner, Hughes & Sutphen, 2008).
This study will add to the existing body of research in knowledge translation. It explores the experiences and views of SSNP occupational therapists to answer the research question how to improve knowledge translation in stroke rehabilitation. The speed and dissemination of research into practice appears to be severely delayed (Hammond, 2005) and in order to allow stroke patients to profit from research as soon as possible, the delivery of new therapy interventions has to happen without delay (Graham, 2006).
This study used a qualitative, descriptive research design to allow the researcher to explore Specialist Section of Neurological Practice (SSNP) Occupational Therapists’ personal experiences and views regarding knowledge translation in stroke rehabilitation. Semi-structured interviews were chosen to allow participants to explore views using open-ended questions and to ensure richness and depth of data (Oppenheim, 1992). Purposive sampling was used recruiting occupational therapists who were members of a specialist interest group for neurological practice. The participants were informed via an invitation email that identity would be kept anonymous, their participation was voluntary and they could terminate participation without giving a reason at any time. The first 8 respondents that fulfilled the inclusion criteria were invited to take part in the study and informed written consent was gained before data collection. Telephone interviews were conducted to allow recruitment of participants from a wide geographical area.
Credibility was ensured by having one participant verifying verbatim notes of interview and developed themes; the detailed description of the interview procedure made transferability possible; the study was dependable as findings were confirmed with literature; bias was avoided by continual verbal and written reflections completed by the researcher. The evaluation points for qualitative research by Hammell et al. (2000) was used, alongsie a qualitative research checklist from the critical appraisal skills program (CASP, 2013).
Ethical approval was granted by the University of Brighton School Research Ethics and Governance Panel (SREGP)..
Inclusion criteria: Participants had to be members of the Specialist Section of Neurological Practice and have at least 2 years’ experience working in stroke rehabilitation. None of the respondents were personally known to the researcher ensuring that there was no coercion possible in the recruitment process, and a power dynamic was avoided (Braun & Clark, 2013).
The thematic analysis by Braun and Clarke (2013) was used including six phases of analysis: familiarization, coding, creating themes, reviewing, defining and naming themes, and finally report writing. The analysis was carried out independently by both the researcher and research supervisor and final themes and categories were agreed.
Nine SSNP members responded to the invitation and seven participated in the study. The participants had between three to ten years experience working with stroke survivors in rehabilitation, three of them had a Bachelor degree and four a Masters qualification.
Following the thematic analysis the main themes identified related to 1) how occupational therapists respond to change; 2) how knowledge translation barriers could be seen as learning needs and as such might lead to empowerment for clinicians and researchers; 3) how the step from knowledge to wisdom and applying KT strategies.
The clinicians’ responses to change such as new therapy interventions can either act as barriers or facilitators of KT. All participants highlighted responses to change as influencing KT in practice, including stress due to time pressure, uncertainty and geographical isolation. Interestingly participants reported both negative and positive responses to change in their practice.
Several participants counted the reasons for stress such as increasing caseload, staff shortages and funding cuts which had direct impact on KT: “…with everybody being so busy trying to see patients that nobody steps back and changes anything…they are just trying to keep their head above water…” (P. 7:262).
Several quotes revealed the uncertainty clinicians have relating personal experience, empirical knowledge, clinical reasoning, and implementing new evidence in their practice: “…as far as I’m concerned the jury is still out on this splinting high tone thing…I have done it with people…who have really benefited…which is great for them…and…ehm…it becomes hard than not to do something…when you know it benefited someone” (P. 4:610).
Some participants mentioned a low motivation towards new interventions and the tendency to resist development as a response to prospective change. This highlights the difficulties some clinicians may experience when trying to link empirical knowledge with the current research evidence, and the complexity of clinical decision making, which KT does not take into account: “…and I think that people get set in their ways…and they are used to…you know…you almost have a little recipe when you have someone with a certain type of impairment and you do the same things all the time and they (clinicians) don’t have to change…ahmmm…so there is some…I guess resistance in a way to change…” (P. 7: 204).
The feeling of isolation was mentioned by three participants, two working in the community and one working in a hospital. For KT to happen the clinician has to be in the place where KT happens, however, this was difficult for some participants: “…yah, a lot of us would like to go on them (relating to cognitive rehabilitation training), but it’s just too far and they are usually two day courses, so you have to have an overnight stay and childcare and all sorts of things…” (P. 5:139).
Interestingly two participants expressed very positive reactions to new knowledge and research evidence. They showed their enthusiasm about new interventions they were introducing into their work with stroke patients: “…one […] excellent study day I went to was by Janice Eng and it is about the GRASP upper limb programme…so that’s another area of practice that we are trying to incorporate…” (P.7:126).
All participants described initiatives used while adapting to change and participants highlighted that identifying and addressing learning needs can lead to empowerment. This is seemingly a new finding on this topic as the researcher could not find related literature which mentioned self-initiative and exploring alternative routes to KT goals. Strategies used by the participants included developing their own implementation guidelines, finding support, and networking. However, barriers to KT identified by the participants included lack of clarity in research evidence and issues related to translation of evidence for a laboratory research setting into the clinical setting.
One participant outlined how an implementation guideline for a new intervention which did not previously exist was created and was disseminated to other teams in the same Trust: “… there has been a lot of work on mirror box therapy specifically and have read lots of research articles and …and…ehm devised a sort of handy…quick user guide and they have made up a kit and we have all of that stored on our share work drive…so we can access it across the whole in-patient OT pathway” (P.2:58).
This is an excellent example in the field of KT as the participant showed initiative in synthesizing, disseminating and exchanging information with others. No literature was found on the initiative of developing own guidelines however, it appears that self-learning can be an efficient tool when implementing new practices without guidelines.
One of the participants initiated fund-raising and recounted several projects being started: “So for example we are looking to develop a […] project, so we’re looking to be firstly […] with an expert charity in that field” (P. 3:243).
Several participants took similar initiative with how they justified the attendance of courses and in-services in occupational therapy departments: “…I think we as practitioners we have kind of…stood by saying: Well, look it’s time well spent, if we spend an hour a month (for in-services)…it’s going to be directly invested in improvement of practice…and better results for our patients…” (P. 5:216).
The researcher agrees that justifying training on the background of professional standards (COT, HCPC, RCP), including the goals of best practice and lifelong learning will support KT by making courses, workshops, and training available to staff.
Many participants highlighted the importance of networking and how this improved knowledge exchange, opportunities for additional training, discovering new interventions and projects, sharing skills, finding support groups, covering supervision needs and linking to academic support: “…we’re also part of the…ehm…district wide…OT Stroke Forum which meets quarterly…all grades and again people share back from training, share evidence-based practice, each time we meet we have a new focus” (P. 2:68).
Some participants stated that articles were too academic and they would prefer more easily understood and less complicated descriptions from researchers: “…so it’s sometimes the evidence is there, but the clarity of the evidence is hard…” (P. 6:559). “…and articles tend to be very academic, and they don’t actually talk about the practical applications…” (P.5:96)
Several participants described situations where the implementation did not work for their patients and that the research lacked information they needed, they did not consider the psycho social needs of the individuals or the resource limitations of the clinical setting. All of these issues were cited as key barriers for KT.
This theme appeared to the author with the realization that knowledge applied in practice is wisdom. This principle was postulated by Ackoff (1989) within the field of systems thinking. It implies the evaluated thinking and according to Ackoff (1989) leads to understanding. Some participants after evaluating and understanding the advantages suggested possible strategies to facilitate KT in practice.
One participant was very knowledgeable in the area of KT strategies and had information about using a KT facilitator or broker to improve KT. However, most participants were not aware of this as a possible strategy: “…but it’s a massive study […]…which just use guidelines and those who have a knowledge broker plus the guideline…looking at outcomes, ‘cause that’s the only way…you know they have to be a big study which says: Oh, look this unit gets people out quicker cause their interventions are better…” (P. 7:647).
This topic relates to the combined effort between academic, researcher and clinician. Several participants mentioned that the research outcomes did not always assist in changing practice and one participant recommended collaborative research: “…they (undergraduates) do a research proposal…with an extensive review…and the university is always saying to us: Tell us what you want…you know …tell us where the gaps are…’ (P. 4:870).
Several participants suggested a role for COT in creating a central website, making articles more easily available and highlighting importance. Five participants supported the idea that the COT could highlight and summarize articles including their relevance and news worthiness but also including any suggested changes to practice: “…but annually some really strong articles saying why we should do one thing and not another…or at least qualify why we are not doing one thing and not another could be generated…that would be helpful…” (P1:56).
Although all participants were aware of the BAOT/COT website and some also knew the Australian (OT-seeker) or Canadian (Stroke-Engine) website they felt the development of a central website as KT pool could result in easier and faster uptake of new interventions when accessing databases.
The NHS is ever-changing and participants all identified responses to change which influenced knowledge translation in practice. Graham et al. (2006) stated that it is an enormous commitment for clinicians to keep up to date with KT despite it being essential to AHPs as it presents part of their professional and regulatory body standards. Stress due to time pressure was identified as a key barrier to KT and Poulsen et al. (2014) made the recommendations that “Educators, clinicians, administrators, and policy makers need to take proactive steps to assist practitioners at risk of burn-out” (p. 163). Gupta et al. (2012) found that there was a direct relationship between ‘unmanageable workload and exhaustion’ (p. 93). The authors recommended coping strategies and workshops to lighten the load of work related stress, including approaching the issue as a team and sharing responsibilities. These findings suggest that time appears to be one of the most significant barriers to knowledge translation and all recommendations to improve KT require time.
Some participants showed uncertainty between knowing about the evidence (Lannin et al, 2007) which recommended not to splint stroke patients with high upper limb tone in general and the participant’s own positive experience of splinting. As a result the new evidence was not implemented into practice. Kilbride et al. (2013) clarified that guidelines for splinting required further research in order to improve KT for splinting in future. Subsequently new splinting guidelines in the UK were published in 2015 (Kilbride et al., 2015).
According to McCluskey et al. (2013), resistance was a more hidden barrier in KT; they pinpointed several requirements for behavioural changes in therapists, which are: beliefs about AHP’s capability and consequences of therapy assessment and intervention, remembering steps and reasoning for interventions, becoming knowledgeable about new interventions and prioritizing new interventions. Appleby and Tempest (2006) highlighted common factors responsible for resistance to change “seeking to protect the status quo, misunderstanding and lack of trust, contradictory assessments and low tolerance for change” (p.477). They reported good results with dissemination and adherence to guidelines following the eight step process of Creating Major Change by Kotter (1996); the steps included 1. Evidence and establishing a sense of urgency, 2. Creating the guiding coalition, 3. Context and developing a vision and strategy, 4. Communicating the vision and strategy, 5. Facilitation and empowering broad-based action, 6. Generating short-term wins, 7. Consolidating gains and producing more change, 8. Anchoring new approaches in the culture. His application of change strategies and developing rehabilitation intervention protocols were important factors for a successful KT strategy in 2006.
Literature exists on occupational therapists working in rural jobs in countries such as Australia, Canada and USA but no literature was found for the UK. Campbell et al. (2012) highlighted poor job satisfaction when having decreased access to professional development and working in professional isolation. The extrinsic factors for job satisfaction were, for example, salary and security, while intrinsic factors were “challenge, autonomy and perceived significance of work” (p. 2). The authors identified in their study that intrinsic factors were rated higher by the AHPs. The solutions recommended by the authors were a combination of extrinsic and intrinsic factors which would increase job satisfaction and decrease job turnover (Campbell, 2012). Poor access to professional development is a barrier to KT and would need to be addressed to support the clinicians.
Accepting the challenge is a facilitator for KT in implementing best practice. Menon et al. (2010) stated that new interventions can be challenging. They explored challenges in the use of rehabilitation guidelines and found that time was the main work place barrier, while confidence in skills was the barrier for clinicians. They identified the rewards as improved knowledge for therapists, improved practice behaviours as well as better outcomes for patients (Menon et al., 2010).
The learning need of finding support can be changed into the empowerment of using support. In an NHS organization for example the League of Friends or the Goodwood Trust are mostly applied to for funding to support courses or projects or other organizations depending on the area. No literature was found which compared NHS and private funding for occupational therapy projects. The initiative mentioned by participant 7 had a fast and direct impact on KT by funding a group project.
Though no articles were found on the topic of networking in stroke rehabilitation, contacts with networks can be realized on the COT (2014) website. Kielhofner in 2005 suggested the idea of ‘Communities of Practice’. He reasoned that clinicians who use knowledge together must also generate knowledge together and by doing so progress knowledge into practice (Kielhofner, 2005). Several participants highlighted that combined effort between clinical practice and education could enhance KT. However, achieving the goal of collaborative research to improve KT is rather complicated in the United Kingdom due to separate accountabilities in patient care, research and education (Ovseiko et al., 2014).
Bosch et al. (2014) indicated that the clarity of evidence was an important factor to researchers and made suggestions for improving clarity which are: specifying intervention definition, clear description of intensity, frequency and duration as well as similar outcome measures for (in this research) upper limb stroke studies. The impact on improving KT is evident as clarity of evidence supports appropriate transfer of knowledge into practice.
Stroke survivors exhibit heterogeneity in practice which impacts on how the clinician can apply new techniques. Kloda et al. (2009) in a literature review investigated the clinical information behaviours of AHPs working in rehabilitation and compared them to physicians. They concluded that AHP’s information behaviour was not much studied and their requirements were poorly known; therefore they suggested further research in the area of AHPs information requirements to be able to apply new interventions in their practice. The improved awareness of clinicians’ requirements may support KT in future.
The topic from knowledge to wisdom became evident in Ackoff (1989), a systems theorist who explained the development from data to wisdom hierarchy, in which he defines wisdom as applied knowledge. One participant introduced research which used clinical guidelines and a knowledge broker. Knowledge brokering is assisting clinicians to make EBP decisions and include knowledge application (Frazer Health, 2009). Bayley et al. (2012) in a study across five stroke rehabilitation centers recruited 79 multidisciplinary team members who were trained in a six month workshop and additionally had a facilitator (broker) to support KT. The results consisted of enhanced clinician implementation skills and improved outcomes for patients which are a perfect example for improved KT.
Di Rezze et al. (2013) used a KT strategy called Summary of Findings (SoFs) in which they gave detailed information of articles regarding risks of a study (comparing intervention group to control group), including details such as the relative effect of the intervention, the sample size, the quality of evidence and a comment section. The results suggested easier application of evidence when using Summary of Findings for clinicians which in turn can improve KT.
This study highlighted that KT is not routinely happening in clinical practice and KT the clinical guidelines are not always followed. KT barriers such as time and resources, attitude and behaviour of clinicians, uncertainty towards research and resistance towards change were identified. These barriers need to be identified in a case by case approach due to variable organizational barriers in each single environment in order to recommend solutions. Training is needed to improve time management skills, coping strategies, assistance through supervision and managerial involvement to prevent workplace burn out. The multiple personal initiatives reported by participants in this study needs to become natural to all occupational therapists and thereby create new areas of occupational therapy innovation. Networking was one initiative which has similarities with communities of practice; this is a means of keeping up to date and ahead of change. Learning needs appear to exist for clinicians as well as for researchers; they require recognition of their learning needs and these are seen as an opportunity for empowerment. Further improvements need to happen giving a wider perspective on EBP and KT. The answers to the key questions would provide better information to clinicians and thereby support correct and easier implementation ,an area that could be influenced by policymakers and publishers of new evidencee. There is a vast field of stakeholders involved in KT and occupational therapists have only a small area they can influence in the KT process, which makes initiative, innovation and involvement even more important.
The data for this study was collected via telephone interviews, this was chosen as the participants lived very far apart and in quite a distance from the researcher, which would have caused high travel expenses. The use of telephone interviews might be of disadvantage and instead opting for Skype interviews would improve the reception of visual cues, gain more contextual information, improve rapport with participants and ensure the possibility of reading body language.
Further topics for future studies were suggested by the author leading into additional investigation of the topic of KT and EBP, into collaborative research amongst separate accountabilities, into improvement of clarity regarding evidence and better application in practice, and into AHP information behaviour.
We gratefully acknowledge the supportive advice provided by Jon Wright (course lead) of the University of Brighton, MSc Health through Occupation.
Appleby, H., & Tempest, S. (2006) Using Change Management Theory to Implement the International Classification of Function, Disability and Health (ICF) in Clinical Practice. British Journal of Occupational Therapy, 69(10), 477:480.
Ackoff, R.L. (1989) From Data to Wisdom. Journal of Applied Systems Analysis, 16:3-9
Bayley, M.T., Hurdowar, A., Richards, C.L., Korner-Bitensky, N., Wood-Daphinee, S., Eng, J.J., McKay-Lyons, M., Harrison, E., Teasell, R., Graham, I.D. (2012) Barriers to implementation of stroke rehabilitation evidence: findings from a multi-site pilot project. Disability and Rehabilitation, 34 (19), 1633-8.
Benner, P., Hughes R.G. & Sutphen, M. (2008). Clinical Reasoning, Decision making, and Action: Thinking Critically and Clinically In Hughes, R.G. (ed) Patient Safety and Quality: An Evidence-Based Handbook for Nurses. Rockville: National Center for Biotechnology Information (NCBI) or other institution of the U.S. government.
Bosch, J., O’Donell, M. J., Berreca, S., Thabane, L., & Wishart, L. (2014). Does Task Oriented Practice Improve Upper Extremity Motor Recovery? A Systematic Review. International Scholarly Research Notice. Retrieved from http://dx.doi.org/10.1155/2014/504910
Braun, V., & Clark, V. (2013) Successful qualitative research: A practical guide for beginners. London: Sage.
Critical Appraisal Skills Program (2013) CASP. Retrieved from http://www.casp-uk.net/#!casp-tools-checklists/c18f8
Campbell, N., McAllister, L., & Eley, D. (2012) The influence of motivation in recruitment and retention of rural and remote allied health professionals: a literature review. Rural and Remote Health, 12, 1900. Retrieved from http://www.rrh.org.au/publishedarticles/article_print_1900.pdf
Christ, P.A. (2010) Adapting Research Instruction to Support the Scholarship of Practice: Practice-Scholar Partnership. Occupational Therapy in Health Care, 24(1):39-55.
Clarke, F., Park, D.J., & Burke, J.P. (2013) Dissemination: Bringing Translational Research to Completion. American Journal of Occupational Therapy, 67(2), 185-193.
Di Rezze, B., Santesso, N., & Law, M. (2013) Exploring the utility of a novel knowledge translation tool for school-based occupational therapists.British Journal of Occupational Therapy, 76(4), 194-99.
Frazer Health (2009) Proven Knowledge Transfer and Exchange Strategies. Retrieved from http://research.fraserhealth.ca/media/2009%20May%2014%20%20Proven%20KTE%20Strategies%20%20%20full%20document.pdf
Graham, I.D. (2006) Lost in Knowledge Translation: Time for a Map? Journal of Continuing Education in The Health Professions, 26(1), 13-24.
Grimshaw, J.M., Eccles, M.P., Lavis, J.N., Hill, S.J., & Squires, J.E. (2012) Knowledge translation of research findings. Implementation Science, 7, 50.
Gupta, S., Paterson, M.L., Lysaght, R.M., & von Zweck, C.M. (2012) Experiences of burnout and coping strategies utilized by occupational therapists. The Canadian Journal of Occupational Therapy, 79(2).
Hammel, K.W., Carpenter, C., & Dyck, I. (2000) Using Qualitative Research. A Practical Introduction for Occupational and Physical Therapists.Toronto: Churchill Livingstone.
Hammond, R., Lennon, S., Walker, M.F., Hoffman, A., Irwin, P., & Lowe, D. (2005) Changing occupational therapy and physiotherapy practice through guidelines and audit in the United Kingdom, Clinical Rehabilitation, 19, 365-371.
Health and Care Processional Council. (2014, p. 14). Retrieved from http://www.hpc-uk.org/assets/documents/10004532Enc08-Consultationonchangestotheprofession-specificstandardsofproficiencyforclinicalscientists.pdf
Huges, A.M., Burridge, J.H., Demain, S.H., Ellis-Hill, C., Meagher, C.,Tedesto-Triccas, L.,Turk, R., & Swain, I. (2014) Translation of evidence-based Assitive Technologies into stroke rehabilitation: users’ perception of barriers and opportunities. BMC Health Services Research, 14, 124.
Jansen, L., Rasekabe, T., & Holland, A.E. (2012) Finding evidence to support practice in allied health: Peers, experience, and the Internet. Journal of Allied Health, 4(4), 154-161.
Kielhofner, G. (2005) Research Concepts in Clinical Scholarship – and Practice: Bridging the divide. American Journal of Occupational Therapy, 59(2), 231-239.
Kilbride, C., Hoffman, K., Tuckey, J., Baird, T., Marston, L., & De Souza, L. (2013) Contemporary splinting practice in the UK for adults with neurological dysfunction: A cross-sectional survey. International Journal of Therapy and Rehabilitation, 20(11), 559-566.
Kilbride C (2015) Updated guidance aims to spread best practice on splinting for contractures. Retrieved from http://www.csp.org.uk/news/2015/01/27/updated-guidance-aims-spread-best-practice-splinting-contractures
Kloda, L.A., & Bartlett, J.C. (2009) Clinical information behaviour of rehabilitation therapists: a review of the research on occupational therapists, physical therapists, and speech-language pathologists. Journal of Medical Librarians Association, 97(3), 194-202.
Klotter, J. (1996) Leading Change. Boston: Harvard Business School Press.
Lannin, N.A., Cusick, A., McCluskey, A., & Herbert, R.D. (2007) Effects of Splinting on Wrist Contructure After Stroke. Stroke, 38, 111-116.
McCluskey, A., & Middleton, S. (2010) Delivering an evidence-based outdoor journey intervention to people with stroke: Barriers and enables experienced by community rehabilitation teams. BMC Health Service Research, 10, 18.
McCluskey A, Vratsistas-Curto A, Schurr K (2013) Barriers and enablers to implementing multiple stroke guideline recommendations: a qualitative study. BMC Health Services Research, 13, 323.
McKenna, K., Bennett, S., Dierselhuise, Z., Hoffman, T., Tooth, L., & McCluskey, (2005) Australian occupational therapists’ use of an online evidence-based practice database (OT seeker). Health Information and Libraries, 22, 205-214.
Menon, A., Bitensky, N.K., & Straus, S. (2010) Best practice use in stroke rehabilitation: from trials and tribulations to solutions! Disability and Rehabilitation, 32(8), 646-649.
Oppenheim, A.N. (1992) Questionnaire Design, Interviewing and Attitude Measurement. London, New York: Continuum.
Ovseiko, P.V., Heitmueller, A., Allen, P., Davies, S.M., Wells, G., Ford, G.A., Darzi, A., & Buchan, A.B. (2014) Improving accountability through alignment: the role of academic health science centres and networks in England. BMC Health Services Research, 14, 24.
Petzold, A., Korner-Bitensky, N., Salbach, N.M., Ahmed, S., Menon, A., & Ogourtsova, T. (2012) Increasing knowledge of best practices for occupational therapists treating post-stroke unilateral spatial neglect: results of a knowledge-translation intervention study. Journal of Rehabilitation Medicine, 44(2), 118-24.
Pomroy VM, Tallis RC, Stitt E (2003) Dismantling Some Barriers to Evidenced-based Rehabilitation with ‘Hands-on’ Clinical Research Secondments. Physiotherapy, 89 5:5
Poulsen, A.A., Meredith, P., Khan, A., Henderson, J., Castrisos, V., & Khan, S.R. (2014) Burnout and work engagement in occupational therapists. British Journal of Occupational Therapy, 77(3), 156-164(9).
Sackett, D.L., Rosenberg, W.M.C., Muir Gray, J.A., Haynes, R.B., & Richardson, W.S. (1996) Evidence based medicine: what it is and what it isn’t. British Medical Journal, 312, 71.
Taylor, M.C. (2000) Evidence-Based Practice for Occupational Therapist. Oxford: Blackwell Science.
Tetroe, J.M., Graham, I.D., Foy, R., Robinson, N., Eccles, M.P., Wensing, M., Durieux, P., Legare, F., Nielson, C.P., Adily, A., Ward, J.E., Porter, C., Shea, B., & Grimshaw, J.M. (2008) Health research funding agencies’ support and promotion of knowledge translation: an international study. The Milbank Quarterly, 86:125-155.
Turner, P.A., & Whitfield, T.W.A. (1996) A multivariate analysis of physiotherapy clinicians’ journal readership. Physiotherapy and Practice, 12, 221-230.
Turner, P.A., & Whitfield, T.W.A. (1997) Physiotherapists’ use of evidence based practice: a cross-national study. Physiotherapy Research International, 2(1), 17-29.
WHO. (2005). Bulletin of the World Health Organization. Knowledge Translation in Global Health. Retrieved from http://www.who.int/bulletin/volumes/83/10/editorial21005html/en/
WHO. (2012). Framework for Ageing and Health. Retrieved from http://www.who.int/ageing/publications/knowledge_translation.pdf
Wilkinson, S.A., Hinchcliffe, F., Hough, J., & Chang, A. (2012) Baseline evidence-based practice use, knowledge, and attitudes of allied health professionals: a survey to inform staff training and organisational change. Journal of Allied Health, 41(4), 177-184.
Wiseman-Hakes C., MacDonald S., Keightley M. (2010) Perspectives on evidence based practice in ABI rehabilitation. “Relevant Research”:Who decides? Neuro Rehabilitation, 26, 355-368.
Jun
21
Osteoarthritis (OA) is the most common degenerative joint disorder. Sufferers of this condition find that it impacts on the quality of their lives (QoL). Exercise is thought to be an important non-pharmacological approach for symptom management.
Aim and Objectives: The purpose of this systematic literature review was to examine the effectiveness of exercise (both land and water based), in improving the QoL of individuals with knee osteoarthritis.
A systematic search was undertaken of AMED, The Cochrane Library, CINAHL, MEDLINE and PEDro along with the Google Scholar databases. The timing of these searches was from September to November 2014. Studies were selected based on pre-set eligibility criteria. Two independent reviewers appraised the selected studies using the PEDro scale and collaborated in order to establish a rigorous perspective on the quality of the research.
From 782 papers initially, 12 studies were included in the review; 10 high quality and 2 moderate quality primary studies and involving a total of 687 participants. The three most common outcome measures used were KOOS (Knee Injury and Osteoarthritis Outcome Score), Nottingham health profile and SF 36. There was strong evidence supporting exercise and physical activity as effective in improving the QoL for people with knee OA based on 8 high and 2 moderate quality studies. The review did not draw any conclusions on the effects of aquatic exercise on QoL due to conflicting evidence. Also noted was conflicting levels of significance under different exercise conditions; significant difference was high when exercise was compared to a non-intervention or education control group and less so when exercise was compared with drug therapies such as NSAID.
Exercise and physical activity, either combined with appropriate drug therapies, or as a single intervention is effective on improving QoL in people with knee OA. However, the most effective exercise dose prescription, the individual aspects of a multicomponent programme, or the additional benefit of a home exercise and walking programme remain uncertain.
Osteoarthritis (OA), a degenerative joint disease, is one of the most common musculoskeletal disorders and represents a major, global public health problem (Alkan et al., 2013). The cause of the disease remains unknown; however, current evidence suggests that it is a result of an interplay of intrinsic and extrinsic risk factors such as old age, female gender, ethnicity, genetic factors, obesity, previous trauma, repetitive use of joints and occupation, which lead to the development of the disease particularly in weight-bearing joints like the knee (Iwamoto et al., 2011). It presents with progressive structural alterations to the joint which includes loss of articular cartilage, osteophytes formation, muscle weakness, and ligamentous laxity (Bennell et al., 2012).
Knee osteoarthritis is the most commonly encountered type, affecting about 18% of women and 9.8% of men globally and its incidence is projected to double by the year 2020, largely due to increased obesity and old age (Johnson and Hunter, 2014; Akinpelu et al., 2009). The disease progression is usually slow and characterised by stiffness, pain, muscle weakness, joint instability and reduced physical functions such as difficulty in walking, stair climbing and squatting, moving from sitting to standing (Yilmaz et al., 2012; Heidari, 2011; Chaipinyo, and Karoonsupcharoen, 2009). In advanced stages pain becomes continuous, muscle atrophy and limb deformity result (Micheal et al., 2010). All such complaints give rise to physical disability which could ultimately lead to restrictions in QoL with time (Yilmaz et al., 2012).
The burden of knee OA does not only include physical problems, but also high economic and social burden largely attributed to the effects of the disability, comorbid diseases, treatment expenses (Bitton, 2009; Woolf and Pfleger, 2003). It also brings with it detrimental psychological effects such as helplessness, coping difficulties and depression, all experienced at higher levels than the general population in people with the condition (Litwic et al., 2013; Cook et al., 2007).
QoL is described as a global construct which includes all aspects of life such as an individual’s perceived position within societal systems and in relation to their expectations and concerns. QoL is reported to be low in people with knee OA with a correlation existing between disease progression and QoL levels dropping significantly compared with other chronic diseases (Farr II et al., 2013; Alves and Bassitt, 2013). It is evidenced that people with OA experience major changes in daily life influenced by the severity of symptoms and impact on functional capacity, affecting their QoL (Chan and Chan, 2011; Egan and Mantes, 2010).
In recent years, QoL has become an important outcome in chronic conditions such as OA where health involving living with and managing one’s condition becomes important (Bernad-Pineda et al., 2014; Phillips et al., 2013; Hoptman et al., 2009). Although not fatal, patients with knee OA are at risk of developing cardiovascular disease due to obesity (Pietrosimone et al., 2014) which could be linked to physical inactivity resulting from chronic pain and restricted joint mobility. Thus, with a progressive disease of multiple risk factors and symptoms, with no known cure and management of patients depending on relief of symptoms, the importance of improving QoL as an endpoint for management needs to be emphasised (Kao et al., 2012; Dias CR et al, 2003).
Management of osteoarthritis has been a combination of different therapies of both pharmacological and non-pharmacological nature. In physiotherapy, a wide range of treatments including exercise and physical activity are used. The treatment of OA is focused on reducing physical disability, controlling pain while lessening the potentially harmful side effects of medicines (Beckwee et al, 2009; Zhang et al., 2007). Exercise is considered as an effective conventional therapy for knee OA symptoms (Fransen and McConnell, 2008). Based on the evidence of a systematic review of guidelines for physical management of osteoarthritis, exercise was among the strongest recommended interventions as first choice conservative treatment particularly for knee OA (Beckwee et al, 2009; Hootman et al., 2003; Larmer et al., 2014; Royal Australian College of General Practitioners, 2009; Veenhof et al., 2012 and Zhang et al., 2008). Systematic reviews have established the benefits of exercise and physical activities in patients with knee OA on outcomes of pain and function (Smith et al., 2014a; Smink et al 2011., Zhang and Jordan, 2010; Fransen and McConnell, 2009a; Fransen and McConnell, 2008b). However, the effects of exercise and physical activity on QoL are not well established and no review undertaken to date.
Primary studies have assessed the effectiveness of exercise and physical activity on QoL in knee OA; some studies report beneficial effects regarding improving general health (Sheth et al., 2014; Multani, 2005; Thorstensson et al., 2005; Dias CR et al., 2003) while other studies established that exercise is ineffective (Ravaud P et al., 2004; Lund et al., 2008). Due to the varying primary evidence it seemed important that a systematic review was conducted with the aim of summarising the evidence of relevant literature and providing more reliable and generalizable conclusions which could be used in clinical practice. Furthermore, identifying therapies that improve quality of life in patients with knee OA may lessen the clinical, economic and social burden of the disease (Farr II et al., 2013).
The review was based on the Center for Reviews and Dissemination guide (CRD 2009) in order to remain focused on the research question and ensure consistency across all aspects of the review, and thereby reduce the risk of bias (Boland et al., 2014; Young and Solomon, 2009). A literature search of AMED, The COCHRANE LIBRARY, CINAHL, MEDLINE and PEDro was conducted in the middle of November 2014. To ensure a comprehensive search, Internet sources of Google Scholar were conducted to make sure that unpublished papers with registered databases were retrieved (CRD, 2009). While the review attempted to minimise publication bias (Greenhalgh et al., 2014), two non-English studies could not be included due to a lack of resources for translation.
To ensure reliability of the decision process, a second reviewer was involved S.M. (CRD, 2009). To minimise selection bias selection criteria was clearly established and studies were included based on their eligibility. The criteria included; quantitative primary studies conducted in English, adult participates with clinically diagnosed knee OA, studies that investigated both knee and hip osteoarthritis, but reported the results separately for each area in order to extract data for knee OA and intervention that included exercise and or physical activity with a control group of alternative interventions. To ensure reliability of the results across studies (Fawcett 2007), only standardized scales were included; SF 36, Short Form SF-36, KOOS (Knee Injury and Osteoarthritis Outcome Score); Nottingham Health Profile (NHP); and other QoL scales. While the review aimed to include different types of quantitative studies other than RCTs in order to ensure a comprehensive review of available evidence, however, only RCTs and one quasi-experimental study met the requirement. In total 12 studies were reviewed as outlined in the flow chart below.
Quality assessment is important to ensure that included studies provided sufficient robustness for the results to be trustworthy and generalisable (Boland et al., 2014). Eleven RCTs and one quasi-experimental study met the inclusion criteria. The PEDro scale (available at www.pedro.org.au) was used to assess the methodological quality (Verhagen et al., 1998). Levels of scores were based on those outlined in a study by Abiebr (2011); study scoring below 4 was low quality, a score of 4-5 was moderate quality and 6-10 was high quality.
Data extraction was undertaken by the author and a reviewer independently. Depending on evidence provided, results on QoL outcomes measures were extracted at two time points; post-treatment and follow-up results and were recorded as short-term (within three months) and long-term follow up (above three months) as shown in tables 2, 3a to 3d below. The reviewers discussed the findings and disagreement was resolved through dialogue.
To comprehensively assess QoL which is a influenced by variables such as age, physical and social functioning, emotional well-being, role activities, perceived health (Rejeski and Mihalko, 2001, Shumaker et al., 1990), results for each subscale were considered as they address these different aspects which ultimately determine QoL for an individual with a chronic disease such as knee OA.
The literature search identified 782 studies; duplicates, unrelated studies were removed and remained with 88 potential studies for initial screening; 9 RCTs and 1 quasi-experimental study with 2 RCTs from reference search were included in the final review. 78 studies did not qualify, thus excluded.

Key: Nottingham Health Profile questionnaire (NHP), verse (vs.), weeks (Wks.). Exercise (Ex), Quasi-Experimental study (Quasi-E)
The quality of the studies is reported in table 2 above, the PEDro score ranged from 4 to 8 and the most common weakness were blinding (therapist, subjects and assessors) and intention to treat analysis. 10 high quality studies scores ranged from 6 to 8 and 2 moderate quality studies scored 4 and 5 respectively.
To further understand the evidence, enhance transparency and prevent errors in interpretation, extracted data for study characteristics and results were tabulated as shown in table 3, 4a, 4b, 4c and 4d below. A total of 687 participants were included. The sample size ranged from n=31 (Aglamis et al 2008) to n=191 (O’Reilly et al., 1999).
The outcomes in tables 4a and 4b show statistical significance found by the authors of the different studies in p-values indicating either significant difference in support of the experimental group or no significant difference between the groups and confidence intervals (95%) with positive values in favour of the experiment group. They are reported according to short- or long-term follow-up for each outcome measure. The duration of interventions ranged from six weeks to six months respectively.
Studies were grouped into physical activity, exercise, aquatic exercise and exercise and physical activity when the interventions were combined, As per protocol, when two interventions were assessed with a control group, the results of one intervention in relation to the control group were reported, thus studies by Wang et al. (2011) and Lund et al. (2010) aquatic exercise were reported, and Evick and Sonel’s (2003) a walking programme instead of exercise was reported. This ensured that the review was inclusive for the type of exercise intervention.
The efficacy of multicomponent strengthening exercises in the management of OA was directly addressed in two high quality studies; Fransen et al., (2001) compared supervised group exercise supplemented with walking to a non-intervention group found significant improvement as reported on the SF 36 scale with the mental component score of CI 2.1 (0.8, 3.4) indicating a narrower confidence interval, and this was without the physical component score reaching statistically significant improvement. Similarly, Thorstensson et al. (2005) conducted a supervised multicomponent exercise complemented with a walking program and found on the SF 36 mental component score (p<0.04) in favour of the intervention.

Key: Combined Results for physical Mental and components (PC + MC), PEDro Score (PS), Exercise (Ex), Verses (vs), standardized response mean (SRM), Results not provided as a combined score
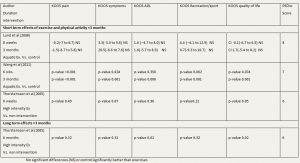
Combined Results for physical Mental and components (PC + MC), PEDro Score (PS), Exercise (Ex), Verses (vs)

Combined Results for physical Mental and components (PC + MC), PEDro Score (PS), Exercise (Ex), Verses (vs)
Dias CR et al., (2003) evaluated the combined effects of walking with supervised progressive concentric-eccentric exercise to a non-intervention group. This moderate quality study reported statistically significant improvement in favour of exercise with functional capacity (p<0.000), physical role (p<0.0004) and general health (p<0.02) on the SF 36 scale. Similar findings were observed in a high-quality study by Aglamis et al., (2008) who reported significant improvement on most subscales of the SF 36 (p<0.001) with effects maintained at both 6 and 12 weeks’ follow-up after a supervised multicomponent functional exercise and walking programme.
Walking versus non-intervention
A moderate quality study by Evcik and Sonel (2002) compared the effects of a 3-month walking programme with a non-intervention group and found statistical and clinical improvement on all subscales of the Nottingham health profile (P<0.001) except for the social isolation dimension.
Exercise alone
Jorge et al. (2015) compared a supervised progressive strengthening programme with a no treatment group and found statistically significant improvement on SF 36 PCS; physical function and physical role (p-value 0.002, p-value 0.002) in favour of the exercise group. The MCS showed no improvement and the control group remained unchanged. While Salli et al. (2010) found that subjects receiving supervised concentric–eccentric exercise showed improvement on outcomes; SF36 PCS (P<0.001) at both 8 and 20 weeks follow-up while on the mental component of the scale, improvement above significant levels showed at 20 weeks follow-up.
Home based strength training
Three high quality studies; investigated the effectiveness of a home based strengthening exercise programme; Baker et al., (2001) compared progressive strengthening with a nutrition education group and evidenced statistically and clinically meaningful improvement in physical function, physical role, social function and mental health (p=0. 01, p<0.009, p<0.012 and p=0. 001) on the SF36 scale. However, the control group showed deterioration in QoL. Similarly, O’Reily et al (1999) conducted home based progressive isometric-isotonic exercises. While improvement was apparent in favour of the exercise, however the results were not significant as shown in table 4b. Doi et al. (2008) assessed home based quadriceps strengthening against non-steroidal anti-inflammatory drugs. Improvement was observed in both groups with positive results in favour of exercise (p<0.001) compared to NSAID (p, 0.023) however the significance difference appeared small. Some of this difference perhaps lies in the issue of motivation to undertake unsupervised exercise involving painful joints.
High quality studies by Wang et al. (2011) and Lund et al. (2008) compared the effects of aquatic exercise involving strength training to non-intervention groups. Outcomes were reported using the KOOS, Wang et al. (2011) found statistical significant improvement on subscales; pain, symptoms, recreation, QoL (p<0.001). Other subscales showed less improvement and the control group remained unchanged. On the contrary, Lund et al. (2008) found no clinical benefits compared with the control group as shown in table 4c, however, the study reported significantly less adverse effects in the aquatic group.
Established on levels of evidence by Tulder et al. (2003) and the incorporated study quality to help interpret results (CRD 2009), findings of 8 high and 2 moderate quality studies provided strong evidence that exercise and physical activities are effective in improving QoL in knee OA. There is inconsistent evidence provided by two high quality studies on the efficacy of aquatic exercise. Overall, evidence from the majority of the studies demonstrated that the interventions could improve QoL with short term effects. Provided below is the table for the level of evidence.
This systematic review summarised evidence from ten high and two moderate quality studies investigating the effectiveness of exercise and physical activity on QoL in knee OA. A number of potential studies were excluded mainly because they were a multimodal management. The review has provided strong evidence from eight high and two moderate quality studies that the interventions could be effective at improving QoL in knee OA. This evidence has established that regular, moderate levels of exercise do not aggravate symptoms in the majority of patients (Messier, 2010; McCarthy and Oldham, 1999). Further, a qualitative study by Wilcox et al. (2006) conducted on perceived exercise benefits, showed improvement, not only on pain and mobility, but also meaningful psychological benefits and enhanced QoL. This could be seen consistent with other studies that found the effects of exercise and physical activity improve self-efficacy and depression, which consequently resulted in improved QoL (Hartman et al., 2000; Penninx et al., (2002); Penninx et al., 2001; Singh et al., 2005; Beckwee et al., 2013)
The effects of strength training on the symptoms of knee OA are supported by wider literature, both of primary and systematic review studies. This is consistent with evidence from other studies that established the benefits of progressive strength training on symptoms in knee OA such as muscle atrophy and weakness which contribute to functional limitations and thereby restrict QoL (Jenkinson et al., 2009; Topp et al., 2002; Jan et al., 2008; Mikesky et al., 2005). Regular supervision as shown in Barker et al. (2001) and Evick and Sonel (2002) seemed to have positively influenced treatment outcome.
Activity is superior to all other treatments in the short term. This review observed that when exercise was compared with a non-intervention group, exercise results were significantly better. Whether this is most effectively performed on land or water remains unclear as included studies provided contradictory evidence. However when activity compared with other treatment groups (e.g. acupuncture), significant differences were small indicating some potential Hawthorne or placebo effects. However it could not be established if the interventions had long-term effects because of the limited number of studies that assessed long-term outcomes.
Overall, studies that included a supervised progressive multicomponent strengthening exercise, supplemented with a home exercise and walking programme found significant improvement in QoL (Jorge et al., 2015; Wang et al., 2011; Aglamis et al., 2008; Thorstensson et al., 2005; Dias CR et al., 2003. Baker et al., 2001; Fransen et al., 2001). This could suggest that physical activities not only provide relief of pain, but also those of psychological and general well-being as well as QoL (Aglamis et al., 2008; Dias CR et al 2003). Which activities are most effective remains uncertain however as Smith et al. (2014b) compared the effects of walking with cycling on QoL in OA knee and found that both groups improved with no statistically significant difference. This may indicate that exercise, although effective, may not be superior to other active interventions in terms of the impact on general wellbeing.
The review included primary studies of high quality and thoroughly reviewed the evidence provided. Publication bias could not be avoided as studies in other languages were removed and studies from less well-known databases may have been missed.
The studies used standardised outcome measures to assess QoL but because they are not specific for measuring QoL in knee OA, they may not adequately assess the area. Based on the PEDro scale, quality studies from moderate to high were included on which evidence was drawn, however, common limitation in the studies was the lack of blinding of participants, therapists and assessors. Some studies had small sample size while some had drop-outs, but did not use intention to treat analysis, which could have impacted on the treatment effects (Joseph et al., 2014) and as a result, may not reflect a true clinical situation.
Clinically this suggests that exercise programmes designed to enhance QoL in knee OA patients ought to target specific impairments such as weakness, as presented in patients (Focht, 2012). This review observed a correlation between pain and QoL. A reduction in pain consequently resulted in improved QoL, thus, knowledge of the interplay of knee OA symptoms on QoL might help in understanding and management of patients. However biopsychosocial factors play a role and related co-morbidities may further complicate the situation (Chan and Wu 2012).
Treatment exercise plans, reinforced with a home exercise/walking programmes could help sustain the effects gained and consequently improve QoL. There is substantial evidence that physical activity has beneficial effects on QoL in knee OA, therefore, could be recommended for patients either as a facility or a home-based programme depending on the patient’s symptoms and preferences. In addition, included studies reported no serious adverse events indicating that moderate regular exercise and physical activity could be safe.
Future research may invest in developing a standardised outcome measure for QoL in knee OA and also developing a knee OA questionnaire assessing facilitators and barriers to exercise as increased understanding of the factors influencing exercise performance in people with OA could help physiotherapists and other health professionals support patients in initiating and maintaining an exercise routine and subsequently improve QoL post initial treatment.
Based on the available evidence, exercise and physical activity appear to be effective in improving knee OA symptoms and QoL. Land based exercise, well supervised home based exercises plus complemented with a walking programme provide significant improvement. Strength training exercises such as eccentric-concentric training provided better results. while exercises alone have short term effects, however, it could be established that these effects could be sustained when exercise and physical activity are incorporated into one’s lifestyle.
Dr Steven May and Mr Mahmoud Saad: Sheffield Hallam University – for guidance and support.
SM as the second article reviewer, many thanks.
ABIEBR, (2011). 1.6 DETERMINING LEVELS OF EVIDENCE. [Online]. Last accessed 21 October 2014 at: http://www.abiebr.com/set/1-introduction-and-methodology/16-determining-levels-evidence.
AGLAMIS B, TORAMAN NF, YAMAN H.The effect of a 12-week supervised multicomponent exercise program on knee OA in Turkish women. J Back Musculoskelet Rehabil2008;21:121–8.
AKERS, J., et al (2009). Systematic review. Centre for reviews and dissemination guidance for undertaking reviews in health care. York publishing service Ltd, USA.
AKINPELU, A., et al (2009). The prevalence of Symptomatic Knee Osteoarthritis in Nigeria. [Online] A Community Community-Based Study. 7, (3) 540-580.
ALKAN, B., ET AL 2014). Quality of life and self-reported disability in patients with knee osteoarthritis, [Online] Modern Rheumatology / The Japan Rheumatism Association, 24, (1), 166-171. Article from Medline EBSCO, Last accessed 25 October 2014 at: http://search.ebscohost.com/login.
ALTMAN, Douglas and BLAND Martine (2005). Statistics Notes: Treatment allocation by minimization. [Online] BMJ: British Medical Journal, 330 (7495), 843.
ALVES, J, and BASSITT, D (2013). Quality of life and functional capacity of elderly women with knee osteoarthritis. [Online] Einstein (São Paulo, Brazil), 11, (2), 209-215.
ANDERSON, C. (2010). Presenting and evaluating qualitative research.[Online]. American Journal of Pharmaceutical Education, 74 (8), 141.
BAKER, K.R., NELSON, M.E., FELSON, D.T., LAYNE, J.E., SARNO, R. and ROUBENOFF, R. (2001). The efficacy of home based progressive strength training in older adults with knee osteoarthritis: a randomized controlled trial. The Journal of rheumatology, 28(7), pp.1655-1665.
BARTOLUCCI, A. and HILLEGASS, W. (2010). Overview, Strength, limitations of systematic review and meta-Analysis. Evidence-Based Practice: Toward Optimizing Clinical Outcomes, 2, 1-8.
BATTERHAM, S.I., et al., (2011). Systematic review and meta-analysis comparing land and aquatic exercise for people with hip or knee arthritis on function, mobility and other health outcomes. BMC musculoskeletal disorders, 12(1), 123.
BECKWÉE, D., et al (2013). Osteoarthritis of the knee: Why does exercise work? A qualitative study of the literature. Ageing research reviews, 12(1), 226-236.
BENNELL K and HINMAN R (2005). Exercise as a treatment for osteoarthritis. Current Opinion in Rheumatology 2005; 17: 634–640
BENNELL, K., et al (2012). Management of osteoarthritis of the knee. [Online] BMJ (Clinical Research Ed.), 345, 4934.
BERNAD-PINEDA, M., et al (2014).Quality of life in patients with knee and hip osteoarthritis. [Online] Revista Española De Cirugía Ortopédica. 58, (5), 283-289.
BITTON, R. (2009). The Economic Burden Of Osteoarthritis. The American Journal Of Managed Care, 15(8), 230-5.
BOUTRON, I. et al., (2007). Reporting methods of blinding in randomized trials assessing nonpharmacological treatments. PLoS medicine, 4(2), 61.
BROSSEAU L, et al (2005). Efficacy of aerobic exercises for osteoarthritis (Part II): A meta-analysis. Physical Therapy Reviews, (9)125–145.
BOLAND A., CHERRY G. and DICKSON R. (2014). Doing a systematic review. A student’s guide. SAGE publication Ltd, London.
BROSSEAU L, et al (2005). Efficacy of aerobic exercises for osteoarthritis (Part II): A meta-analysis. Physical Therapy Reviews, (9)125–145.
CHACÓN, J.G. et al., (2004). Effect of knee osteoarthritis on the perception of quality of life in Venezuelan patients. Arthritis and rheumatism, 51(3) 377–82.
CHAIPINYO, Kanda and KAROONSUPCHAROEN, Orapin (2009). No difference between home-based strength training and home-based balance training on pain in patients with knee osteoarthritis: a randomized trial. [Online] The Australian Journal of Physiotherapy, 55, (1), 25-30.
CHAN, K. K. and CHAN, L. W. (2011). A qualitative study on patients with knee osteoarthritis to evaluate the influence of different pain patterns on patients’ quality of life and to find out patients’ interpretation and coping strategies for the disease. Rheumatology Reports, 3(1), 3.
CHAN, K. and WU, R. (2012). Symptoms, Signs and Quality of Life (QoL) in Osteoarthritis (OA). [Online] Principles of Osteoarthritis. Article from Medline EBSCO, last accessed 4 October 2014 at: http://search.ebscohost.com/login.
CLAUDE, B., et al (2007). Physical activity and health. Human Kinetics Publisher, Leeds.
COOK, C., et al (2007). Osteoarthritis and the impact on quality of life, health indicators. Rheumatology International, 27, (4), 315-321.
CENTRE FOR REVIEWS AND DISSEMINATION (2009). Evidence based guidelines and current practice for physiotherapy management of knee osteoarthritis Research articles Research articles. 745–56.
CROWTHER, David (2013). A clinician’s guide to systematic reviews. [Online] Nutrition in clinical practice: official publication of the American Society for Parenteral and Enteral Nutrition, 28 (4), 459–62.
DIAS, C. R., DIAS, D.J.M. and RAMOS, L.R., 2003. Impact of an exercise and walking protocol on quality of life for elderly people with OA of the knee. Physiotherapy Research International, 8(3), pp.121-130. Last accessed at: http://doi.wiley.com/
DOI, T., AKAI, M., FUJINO, K., IWAYA, T., KUROSAWA, H., HAYASHI, K. and MARUI, E., (2008). Effect of home exercise of quadriceps on knee osteoarthritis compared with nonsteroidal antiinflammatory drugs: a randomized controlled trial. American Journal of Physical Medicine & Rehabilitation, 87(4), pp.258-269.
EGAN, B. and MENTES, J. (2010). Benefits of physical activity for knee osteoarthritis: a brief review. [Online] Journal of Gerontological Nursing, 36, (9), 9-14.
ESCALANTE, Y. et al., (2010). Physical exercise and reduction of pain in adults with lower limb osteoarthritis: a systematic review. Journal of back and musculoskeletal rehabilitation, 23(4)175–86.
ESSER, S. and BAILEY, A., (2011). Effects of exercise and physical activity on knee osteoarthritis. Current pain and headache reports, 15(6), 423–30.
EVCIK, D. and SONEL, B., (2002). Effectiveness of a home-based exercise therapy and walking program on osteoarthritis of the knee. Rheumatology international, 22(3), pp.103-106.
FARR II, J., et al (2013). Quality of life in patients with knee osteoarthritis: a commentary on nonsurgical and surgical treatments. [Online]The Open Orthopaedics Journal, 7, 619-623.
FARROKHI, S. and FITZGERALD, G.K., (2012). The Role of Physical Activity and Therapeutic Exercise in Development and Management of Knee Osteoarthritis. , 19(1), pp.27–36.
FOCHT BC, (2006). Effectiveness of exercise interventions in reducing pain symptoms among older adults with knee osteoarthritis: a review, (14)212–35.
FRANSEN, M., CROSBIE, J. and EDMONDS, J. (2001). Physical therapy is effective for patients with osteoarthritis of the knee: a randomized controlled clinical trial. The Journal of rheumatology, 28(1), pp.156-164.
FRANSEN M., et al (2002).Therapeutic exercise for people with osteoarthritis of the hip or knee. A systematic review. J Rheumatol, (29)1737-45.
FRANSEN, M. et al., (2011). The epidemiology of osteoarthritis in Asia. [Online] International journal of rheumatic diseases, 14 (2)113–21
FRANSEN, M. & MCCONNELL, S., (2008). Exercise for osteoarthritis of the knee. Cochrane Database Syst Rev, (4). Accessed October 25, 2014.
JENKINSON CM. et al. (2009). Effects of dietary intervention and quadriceps strengthening exercises on pain and function in overweight people with knee pain: randomised controlled trial. BMJ, 339(3)170.
JORGE, R.T.B., SOUZA, M.C.D., CHIARI, A., JONES, A., FERNANDES, A.D.R.C., JÚNIOR, I.L. and NATOUR, J., (2015). Progressive resistance exercise in women with osteoarthritis of the knee: a randomized controlled trial. Clinical rehabilitation, 29(3), pp.234-243.
JOSEPH, R. et al., (2015). A systematic review finds variable use of the intention-to-treat principle in musculoskeletal randomized controlled trials with missing data. Journal of clinical epidemiology, 68(1), 15–24.
HEARN, J. et al., (1999). Issues in research: Systematic reviews. Palliative Medicine, 13(1), 75–80.
HEIDARI, B., (2011). Knee osteoarthritis prevalence, risk factors, pathogenesis and features: Part I, Caspian Journal Of Internal Medicine, 2, (2), 205-212.
HURLEY M.V. (2003). Muscle dysfunction and effective rehabilitation of knee osteoarthritis outcomes: What we need to find out. Arthritis Rheum.
GLASGOW, R. E., et al (2003). Why don’t we see more translation of health promotion research to practice? Rethinking the efficacy-to-effectiveness transition. American Journal of Public Health, 93(8), 1261-1267.
GREENHALGH, T. (2014). How to read a paper: the basis of evidence based medicine. 5th ed, Chichester, Wiley.
GUPTA, S. K. (2011). Intention-to-treat concept: A review. Perspectives in clinical research, 2(3), 109.
HIGGINS, Julia and GREEN, Sally (2008). Cochrane handbook for systematic reviews of interventions. Chichester: Wiley-Blackwell.
HOPMAN, W., et al (2009). Associations between chronic disease, age and physical and mental health status. [Online] Chronic Disease in Canada, 29 (2), 108–117.
LIBERATI, A. et al., (2009). The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. [Online] Medicine, 6 (7), 100.
LUND, H., WEILE, U., CHRISTENSEN, R., ROSTOCK, B., DOWNEY, A., BARTELS, E.M., DANNESKIOLD-SAMSØE, B. and BLIDDAL, H., (2008). A randomized controlled trial of aquatic and land-based exercise in patients with knee osteoarthritis. Journal of rehabilitation medicine, 40(2), pp.137-144.
JAN MH. et al (2008). Investigation of clinical effects of high and low-resistance training for patients with knee osteoarthritis: a randomized controlled trial, 88(4):427–36. 57.
JOHNSON, V., and HUNTER, D. (2014).The epidemiology of osteoarthritis. [Online] Best Practice & Research. Clinical Rheumatology, 28, (1), 5-15.
KHAN, K and KUNZ, R, (2011). Systematic reviews. To support evidence based medicine. 2nd edition. Hodder & Stoughton Ltd. UK.
KAO, M., et al (2012).The effectiveness of a self-management program on quality of life for knee osteoarthritis (OA) patients, [Online] Archives Of Gerontology And Geriatrics, 54, 2, pp. 317-324.
LANGE, A.K., et al (2008). Strength training for treatment of osteoarthritis of the knee: a systematic review. Arthritis and rheumatism, 59(10), 1488–94.
LARMER, P., et al (2014). Systematic review of guidelines for the physical management of osteoarthritis, [Online] Archives of Physical Medicine and Rehabilitation, 95, 2, pp. 375-389.
LAVER-FAWCETT, A. (2007). Principles of assessment and outcome measurement for occupational therapists and physiotherapists: theory, skills and application. John Wiley & Sons Ltd, London.
LITTLEWOOD C. and MAY, S. (2013). Understanding Physiotherapy Research. Newcastle, Cambridge Scholars Publishing.
LITWIC, A., et al (2013). Epidemiology and burden of osteoarthritis. [Online] British Medical Bulletin, 105, 185-199.
MAHER, C. G., et al (2003). Reliability of the PEDro scale for rating quality of randomized controlled trials. Physical therapy, 83(8), 713-721.
MAJANI, G., et al (2005). Subjective impact of osteoarthritis flare-ups on patients’ quality of life. Health and quality of life outcomes, 3, .14.
MANNINEN, P. et al., (2001). Physical exercise and risk of severe knee osteoarthritis requiring arthroplasty. 432–437.
MCCARTHY CJ and OLDHAM JA (1999). The effectiveness of exercise in the treatment of osteoarthritic knees: a critical review. Phys TherRev 1999; 4:241–50
MESSIER, S. P. (2010). Diet and exercise for obese adults with knee osteoarthritis. Clinics in geriatric medicine, 26(3), 461.
MICHAEL, J., et al (2010). The epidemiology, aetiology, diagnosis, and treatment of osteoarthritis of the knee. [Online] Deutsches Aerzteblatt International. 107, (16), 294.
MIKESKY AE., et al (2006). Effects of strength training on the incidence and progression of knee osteoarthritis. Arthritis Care Res. 55(5):690–9.59.
MOHER, D., et al (2012). CONSORT 2010 explanation and elaboration: Updated guidelines for reporting parallel group randomized trials. [Online] International Journal of Surgery, 10 (1), 28-55.
MULTANI NK (2005). The changing role of Physiotherapists in the management of osteoarthritis knee, “Physiotherapy”. The Journal of The Indian Association of Physiotherapist,(1)15-20.
NAJAFABADI, M.T et al., (2014). Asian Journal of Multidisciplinary Studies Available online at www.ajms.co.in Comparison of isometric and Pilates exercises on Knee pain and quality of life in women with Knee Osteoarthritis. , 2(3), pp.109–112.
NGUYEN, U., et al (2011). Increasing prevalence of knee pain and symptomatic knee osteoarthritis. [Online] Annals of Internal Medicine, 155 (11) 725-732,
NIGHTINGALE, A. (2009). A guide to systematic literature reviews. Surgery (oxford), 27 (9), 381-384.
O’REILLY, S.C., MUIR, K.R. and DOHERTY, M., (1999). Effectiveness of home exercise on pain and disability from osteoarthritis of the knee: a randomised controlled trial. Annals of the Rheumatic Diseases, 58(1), pp.15-19.
PAGE, M., et al (2014). Bias due to selective inclusion and reporting of outcomes and analyses in systematic reviews of randomized trials of healthcare interventions, The Cochrane Database Of Systematic Reviews, 10, 35.
PELLAND, L. et al., (2004). Efficacy of strengthening exercises for osteoarthritis. Physical Therapy Reviews 9: 77–108
PENNINX B.J., et al (2001). Physical Exercise and the Prevention Disability in Activities of Daily Living in Older Persons With Osteoarthritis, (161)2309-16.
PENNINX, B.W., et al (2002). Exercise and depressive symptoms: a comparison of aerobic and resistance exercise effects on emotional and physical function in older persons with high and low depressive symptomatology. Journals of Gerontology, 57, 124–132.
PETURSDOTTIR, U., et al (2010). Facilitators and barriers to exercising among people with osteoarthritis: a phenomenological study. Physical therapy, 90(7), 1014–25.
PHILLIPS, S., et al (2013). Physical activity and quality of life in older adults: an 18-month panel analysis. [Online] Quality Of Life Research: An International Journal Of Quality Of Life Aspects Of Treatment, Care And Rehabilitation, 22, (7), 1647-1654,
PIETROSIMONE, B., et al (2014). Association between quadriceps strength and self-reported physical activity in people with knee osteoarthritis, [Online] International Journal of Sports Physical Therapy, 9, (3), 320-328.
REJESKI, W. J., AND MIHALKO, S. L. (2001). Physical activity and quality of life in older adults. The Journals of Gerontology Series A: Biological Sciences and Medical Sciences, 56(2), 23-35.
RIDDLE, D.L., et al (2011). Psychological health impact on 2-year changes in pain and function in persons with knee pain: data from the osteoarthritis initiative. Osteoarthritis and cartilage/OARS. Osteoarthritis Research Society, 19, 1095–1101.
ROTONDI, M. and DONNER, A., (2012). Sample size estimation in cluster randomized trials: An evidence-based perspective. Computational Statistics & Data Analysis, 56(5), 1174–1187.
SACKETT, D. L. and WENNBERG, J. E. (1997). Choosing the best research design for each question. BMJ, 315 (7123), 1636.
SALLIi, A., SAHIN, N., BASKENT, A. and UGURLU, H., (2010). The effect of two exercise programs on various functional outcome measures in patients with osteoarthritis of the knee: A randomized controlled clinical trial. Isokinetics and Exercise Science, 18(4), pp.201-209.
SHERRINGTON, C., et al (2003). Reliability of the PEDro scale for rating quality of randomized controlled trials. Physical therapy, 83(8), 713-721.
SHUMAKER SA, et al (1990). Psychological tests and scales. Quality of Life Assessments in Clinical Trials. New York: Raven Press.
SILVA, L.E. et al., (2008). Hydrotherapy versus conventional land-based exercise for the management of patients with osteoarthritis of the knee: a randomized clinical trial. Physical therapy, 88(1), 12–21.
SINGH, N.A., et al (2005). A randomized controlled trial of high versus low intensity weight training versus general practitioner care for clinical depression in older adults. The Journals of Gerontology, (60), 768–776.
SMINK, A., et al (2011).”Beating osteoarthritis”: development of a stepped care strategy to optimize utilization and timing of non-surgical treatment modalities for patients with hip or knee osteoarthritis, [Online] Clinical Rheumatology, 30, (12), 1623-1629.
SMITH, T., et al (2014a). A systematic review to determine the optimal type and dosage of land-based exercises for treating knee osteoarthritis.[Online] Physical Therapy Reviews, 19 (2),105-113.
SMITH, T., et al (2014b). Living with osteoarthritis: a systematic review and meta-ethnography, Scandinavian Journal of Rheumatology, 1-12.
TALBOT LA., et al (2003). A home-based pedometer-driven walking program to increase physical activity in older adults with osteoarthritis of the knee: A preliminary study. J Am Geriatric, 51(3)387–392.
THOMAS K, et al (2002). Home based exercise programme for knee pain and knee osteoarthritis: randomised controlled trial. BMJ, (325)752–5.
THORSTENSSON, C.A., ROOS, E.M., PETERSSON, I.F. and EKDAHL, C., (2005). Six-week high-intensity exercise program for middle-aged patients with knee osteoarthritis: a randomized controlled trial [ISRCTN20244858]. BMC Musculoskeletal Disorders, 6(1), p.27.
TOPP R., et al (2002). The effect of dynamic versus isometric resistance training on pain and functioning among adults with osteoarthritis of the knee. Arch Phys Med Rehab, 83:1187–95.
VEENHOF, C., et al (2012). Factors associated with physical activity in patients with osteoarthritis of the hip or knee: a systematic review, Osteoarthritis and Cartilage / OARS, Osteoarthritis Research Society, 20, (1), 6-12.
VENNU, V., and BINDAWAS, S. (2014). Relationship between falls, knee osteoarthritis, and health-related quality of life: data from the Osteoarthritis Initiative study, Clinical Interventions in Aging, 9, 793-800.
YILMAZ, H., et al (2013). Effectiveness of home exercise program in patients with knee osteoarthritis. European Journal of General Medicine, 10, (2), 102-107.
YOUNG, Jane and SOLOMON, Michael (2009). How to critically appraise an article. Nature Clinical Practice. Gastroenterology & Hepatology, 6 (2), 82-91.
WANG, T.J., LEE, S.C., LIANG, S.Y., TUNG, H.H., WU, S.F.V. and LIN, Y.P., (2011). Comparing the efficacy of aquatic exercises and land‐based exercises for patients with knee osteoarthritis. Journal of clinical nursing, 20(17‐18), pp.2609-2622.
WILCOX, S. et al., (2006). Perceived exercise barriers, enablers, and benefits among exercising and nonexercising adults with arthritis: results from a qualitative study. Arthritis and rheumatism, 55(4), 616–27.
WOOLF, A.D. and PFLEGER, B., (2010). Burden of major musculoskeletal conditions. 81(03).
WORLD HEALTH ORGANISATION (2010). Definition of physical activities. [Online] last accessed 25 October 2014 at: http://www.who.int/topics/physical_activity/en/
ZHANG, C., et al. (2008). OARSI recommendations for the management of hip and knee osteoarthritis, Part II: OARSI evidence-based, expert consensus guidelines Osteoarthritis and Cartilage / OARS, Osteoarthritis Research Society, 16 (12), 1585-1589.
ZHANG, Y. and JORDAN, J. (2010). Epidemiology of osteoarthritis. Rheumatic Diseases Clinics of North America, 34 (3) 515-529.
ZAZA, S., et al (2000). Data collection instrument and procedure for systematic reviews in the Guide to Community Preventive Services. Task Force on Community Preventive Services, [Online] American Journal of Preventive Medicine, 18, (1) 44-74.
Jun
21
Background: Sensory integration techniques which follow the theory outlined by Ayres (1972) are widely used by occupational therapists as an intervention for children and young adults with learning disabilities, but their efficacy is unclear. Research studies have suggested increased levels of participation and other positive behavioural changes following group sessions using sensory integration techniques, but literature reviews have highlighted a scarcity of evidence supporting their use.
Materials and Methods: A qualitative study in which therapy and teaching staff of children and young adults with learning disabilities aged between 5 and 22, at a school and a college in England, were interviewed to gain understanding of their perceptions of the impact of these groups.
Findings: Groups involving sensory integration techniques were perceived to have a positive effect on the abilities and participation (in both the group itself and subsequent learning and other activities) of children and young adults with learning disabilities and other complex needs in educational settings.
Conclusions: The findings are of relevance to occupational therapists and others working with young people with learning disabilities in special educational and other settings. In particular, they suggest variables that may have the potential to be measured in future research evaluating such sensory integration groups.
This article describes research exploring teachers’ and therapists’ perceptions of the impact from children and young adults’ participation in occupational therapy sensory integration groups. Sensory integration theory seeks to explain how an individual organises sensation for use in everyday activities. It was originally developed by Ayres (1972) who investigated how perception, adaptation and learning may be affected by disruption to sensory input. Her theory proposed that the brain assimilates, organises, processes and interprets information from the senses allowing individuals to adapt and interact appropriately with the environment. This promotes optimal functioning, including participation in activity and regulation of behaviour (Ayres, 2005, Watling and Deitz, 2007, Smith et al., 2009). Sensory integration is both a theory and an intervention approach with individuals and groups.
The scope and prevalence of sensory integrative problems may be concerning for families, therapists and teaching staff of young people with learning disabilities, autism and other complex needs. People with learning disabilities have a significantly reduced ability to understand new or complex information, to learn new skills and to cope independently, which starts before adulthood and therefore has a lasting impact on development (Department of Health, 2001). People on the autistic spectrum may behave in restrictive or repetitive ways and experience social or communication difficulties. Individuals with either diagnosis who additionally have sensory-integrative problems may find it challenging to take in and interpret sensory input from the environment, discriminate between different sensations, self-regulate behaviour, maintain posture, use both sides of the body together, sequence activities and plan movement (Bundy, Lane and Murray, 2002, Urwin and Ballinger, 2005, Miller, 2007). Physical, psychological and social impacts are highlighted in the literature (May-Benson and Koomar, 2010, Polatajko and Cantlin, 2010). Quality of life can be severely disrupted, with long term impact on health and wellbeing into adulthood, including social isolation, depression, anxiety and dependence on specialist care (College of Occupational Therapists, 2012).
To address this, Ayres (1972) proposes occupational therapy with a sensory integrative approach on an individual basis from appropriately trained therapists. Many occupational therapists adapt aspects of the original neuro-science theory to make it more relevant for their setting (Smith Roley et al., 2009), for example, running groups rather than individual sessions.
A search of the literature revealed 26 studies related to occupational therapy using a sensory integration approach to promote participation by children or adults with sensory-integrative problems. Three were based in the United Kingdom, one in Canada and the remainder in the United States. All considered children except for one which related to ‘children and adolescents’ and two concerning adults. There were a variety of study designs: systematic or other literature reviews; phenomenological or other qualitative studies seeking the perspectives of parents or teachers; and quantitative research, including single and multiple-subject case studies and longitudinal studies.
The literature suggests that sensory-integrative approaches are widely practiced by occupational therapists with children (and to a lesser extent adults) with sensory processing problems, including those with learning disabilities (Cohn, 2001) and autism (Watling and Deitz, 2007). A number of studies have reported positive impacts, for example:
There are, however, limitations with much of this research and reviews have cautioned about the conclusions that can be drawn from it (May-Benson and Koomar, 2010). The majority of the literature focuses on school-age children and few studies are from the UK. Sample sizes are generally small and the heterogeneity of individuals with sensory integrative problems means that studies have often focused on particular diagnoses, though limited description of participant characteristics often makes comparison between studies difficult. For example, in the studies reviewed by Lang et al. (2012), most participants were diagnosed with autistic spectrum disorders, however, insufficient information was provided to determine if they also had learning disabilities. Isolation of the impact of sensory integration is often absent, with many participants also receiving additional therapy, for example behavioural or speech and language interventions. As a result of the limitations with the existing evidence base, some question whether it is appropriate for sensory integration interventions to be so widely used (Lang et al., 2012).
Changes following sensory integration groups are suggested to support participation in subsequent learning and other activities (Watling and Deitz, 2007), but few studies have measured such changes in participation. As this is key to development and impacts on health and wellbeing, it could be explored further to inform practice (Cribbin and Lynch, 2014). Watling and Deitz’s qualitative study (2007) demonstrates the potential of staff and caregiver perspectives to provide some insight into changes in participation following sensory integration interventions, in contrast to questionnaires which may have restricted parents, teachers and occupational therapists in articulating their opinions (Stonefelt and Stein, 1998).
Although there is suggestion of positive impact from sensory integration groups, the exact nature of this could be clearer, which makes it challenging to measure. This research therefore aimed to explore how occupational therapists, teachers and teaching assistants working with children and young-adult learners perceived sensory integration groups to impact on the participation of children and young adults with learning disabilities.
Qualitative research was completed by the first and second authors involving interviews with therapy and teaching staff at a special educational needs school and college for children and young people aged 5-19 and 18-23 years respectively. Both settings supported children and young people with complex needs including autism, speech and language difficulties, developmental delay and moderate-to-severe learning disabilities. The first author had previously undertaken a student placement in the school, but the authors had no other connection with either setting. The research explored teaching and therapy staff perceptions of the efficacy of the sensory integration groups, in which a number of learners took part, providing insight into some of the complexities of participation for young people experiencing altered sensory needs. It aimed to suggest appropriate variables that could be measured in future evaluations of such groups.
Participant information sheets outlining the study purpose were distributed to eligible participants via the therapy management teams at both settings. Staff were sought who were sufficiently familiar with learners’ usual behaviour to notice any impacts of participating in sensory integration groups (for example, from working directly with them on the same day as the sensory integration group). Different professions were sought as suggested by Doig et al. (2008) and four occupational therapists, two senior teaching assistants and a speech and language therapist volunteered. There were seven participants in total and the workplace of each is given in brackets following their pseudonyms, which are used to maintain anonymity. Sally (School) is a senior occupational therapist with over ten years’ experience working with children with learning disabilities. Jane (School) is an occupational therapist with one years’ experience. Fiona (College) and Rachel (College) are both occupational therapists working at the college for over four years. These occupational therapists themselves ran the sensory integration groups in which 5-6 learners (in the college) and 5-10 learners (in the school) took part. They demonstrated deeper understanding of the purpose and techniques used in the groups. The other participants were familiar with those taking part in the groups and had worked with them in other roles providing therapeutic intervention, teaching or teaching support: Felicity (School), a speech and language therapist with over four years’ experience; Pauline (School) and Emma (College), teaching assistants with over two years’ experience.
Semi-structured individual interviews allowed for flexible data collection as participants were able to discuss learners of their choice. Participants were asked to discuss their perceptions of any effects on engagement or participation that they had observed following sensory integration groups. They were requested not to disclose information which might compromise the anonymity of learners discussed.
Questions explored participants’ understandings of the purpose of the groups and the reasons for learners’ referrals. They were asked to focus upon participation difficulties visible prior to the groups and then encouraged to describe any changes in behaviour, participation or engagement in daily activities they may have subsequently observed, whether during, immediately following the sensory integration groups, or longer-term. Participants were also asked to consider current evaluation methods or methods of gaining feedback from stakeholders to offer insight into outcome measurement. Each interview was transcribed verbatim. Ethical approval was granted by the University of Brighton School of Health Sciences Research and Governance Panel.
The theoretical flexibility and clear stages of thematic analysis gave guidance and structure to data analysis (Braun and Clark, 2013). Themes were identified in the data by identifying repeated ideas, terms, phrases or words between the participants. An inductive approach allowed findings to emerge from the raw data rather than prior expectations. All data was given equal attention, allowing for unanticipated insights and adding credibility. Data from the school was coded by the first author by hand whilst data from the college was coded by the second author with assistance of qualitative data analysis software. Braun and Clark (2013) describe how analysis in this method will be influenced by the knowledge, viewpoint and epistemology of these authors, whose positive perceptions of sensory integration from previous observations risked influencing analysis. They were therefore mindful of this and reflexive in order to minimise this risk by placing equal emphasis on data that was not supportive of its efficacy. Keeping reflexive diaries to explore presuppositions and the analytic process contributed to trustworthiness (Banner, 2010).
The findings relate to perceived changes in behaviour and participation in learning and other activities of young adults and children with learning disabilities, from participating in occupational therapy sensory integration groups at two specialist educational settings.
Rachel (Occupational Therapist, College) described the adult learners as:
“…quite low in their functioning, developmental delay…minimal or non-verbal…not very confident with their own body and their non-execution of certain movements.”
Sally (Occupational Therapist, School) summarised the child learners:
“…social difficulties, difficulties concentrating, difficulties engaging in work, difficulties regulating sensory input…can be sensory seeking.”
The occupational therapists described the groups in detail. In the school, learners were timetabled to attend a daily sensory integration group which had been running since the start of the academic year (around 7 months) and consisted of three ordered stages of activity. Each stage involved the use of different sensory-based equipment to facilitate alerting, organising and calming activities. The activities included the use of therapy balls, swings, skateboards and rope, beanbags and sensory-based soft play equipment. The specific activities and specialist equipment were described as promoting sensory input to stimulate the central nervous system. Following Ayres (2005) this was described as enabling individuals to better-regulate their responses to the environment. Learners also attended individual sessions using a sensory integrative approach which often used one or two of the sensory-based activities from the group.
In the college sensory integration groups were staged for one hour per week and had been running for around 18 months. Similar techniques aimed to improve motor skills, body awareness, planning and execution and to enable identification of behavioural areas of strength or behaviours impacting on learning, for example, problems with waiting or taking turns. These groups involved the same five learners.
Sally (Occupational Therapist, School) described activities as alerting, organising and calming, completed in that order and Fiona (Occupational Therapist, College) explained the set routine of ‘alerting’ activities followed by stimulation of a pre-selected sense (such as taste or touch) and finishing with a period of relaxation. Alerting activities included bouncing on balls or wafting a parachute as a group. Rachel (Occupational Therapist, College) clarified that relaxation might involve weighted blankets, bean bags, listening to music or using ‘sensory baskets’:
“….I rock [the cushion on which he is laying] slowly or he quite likes to have a duvet cover over him…shutting out all the sensory information…..the result is that when he leaves he’s much better in terms of his ability to engage with classroom requests” (Sally, Occupational Therapist, School).
Two overlapping themes were identified: perceived changes in performance capacity and perceived changes in participation following the groups, though participants described their uncertainty as to the extent to which these changes could confidently be attributed to the groups.
Participants described how the groups supported individuals’ ability by impacting upon arousal level, attention, awareness, motor planning and cognitive functioning. It was suggested that sensory integration groups promoted the regulation of very high or very low arousal levels seen in children and adults with learning disabilities, autism and developmental delay, thereby improving levels of participation (see second theme). Emma (Teaching Assistant, College) described the learners as being:
“under responsive and … [having] a really low arousal level…They need sensory input… for regulation, to get them ready to go…”
Sally, (Occupational Therapist, School) explained how sensory integrative interventions provided sensory input into an ‘under responsive system’ and enabled the learners to be sufficiently alert for further therapeutic input.
Participants spoke of how learners could be over or under responsive to their environment, causing an imbalance in arousal levels, interrupting participation:
“He’ll jump and jump….you know he’s in that high arousal state and he needs bringing down with heavier input really to get him ready to attend.” (Jane OT)
The ways they perceived the groups to increase participation in learning activities are further explored within the second theme. In both settings, participants considered the groups to have an immediate impact on, for example, sustained attention and appropriate behaviour:
“…to give some intense vestibular input…..to get that sensory system working…..you can see the difference in five minutes he becomes alert…I can then work on different interventions” (Sally, OT).
Sally (Occupational Therapist, School) described a learner “engaging for longer during the sessions, being able to participate for the whole session.” School participants spoke of visible changes of a short duration, with increased focus lasting for fifteen or thirty minutes, though Jane (Occupational Therapist, School) described the sensory integration groups supporting learners to get ready for a subsequent learning or other activity, because they were then more alert and able to concentrate.
The majority of learners discussed were described as experiencing physical and cognitive difficulties interrupting participation in learning activities, including motor planning, balance problems and gravitational insecurity. Participants referred to improved co-ordination amongst learners, with Rachel (Occupational Therapist, College) considering one learner to have ‘developed a sense of body awareness’ enabling a better regulation of force and control or movements. As a result, they learned to throw gently or slowly, rather than forcefully or aggressively, with Fiona (Occupational Therapist, College) regarding this as helping social development, as such behaviour ‘would frighten people’.
This theme highlights how sensory integration groups are considered to impact on an individuals’ underlying abilities to complete an activity. The second theme explores how these impacts may impact on behaviour and participation in activities.
Participants described changes they had observed in the behaviour and participation of five adult and six child learners within the sensory integration groups. No reference was made to learners’ behaviour remaining unchanged, nor to any aspects of the groups considered by participants or others to be negative.
The groups were described as seeming meaningful for group participants as they were able to complete them in a fun and enjoyable way with others, impacting on self-efficacy, confidence and social interactions. Emma (Teaching Assistant, College) described one learner as initially reluctant to engage, initially needing ‘coaxing or persuading’, but he appeared, to learn to view the groups as a positive environment, participating willingly, which she considered to be “him saying that ‘I’m happy to be here’”. Feedback received from a teacher was also reported; “that he is a lot better after a relaxation session.” She went on to describe another learner who slowly increased time spent in the group, and whose achievement of a target to remain for ten minutes, suggests that the groups resulted in increased participation. Fiona (Occupational Therapist, College) described a different learner:
“…(initially) he would come in for five minutes…he wouldn’t come in at all… and accessed almost the whole session today.”
Participants in the school described the behavioural, learning and sensory needs of the children and their difficulty with self-expression. They explored how the sensory integration groups met these needs and were adapted for optimal participation. Participants in the college felt the groups may have impacted positively on behaviours which enabled increased participation in activities, including reduced aggression and prompting. Emma (Teaching Assistant, College) referred to one learner’s greatly improved ability to wait for their turn (for example for the trampoline) during the groups.
Changes in confidence and communication were referred to frequently throughout the interviews. Fiona (Occupational Therapist, College) described a learner now entering the room confidently and willingly and alternating between activities more independently. This learner also displayed increased independence by flushing the toilet with confidence which had not happened previously. The sensory integration groups were also thought to support development of peer relationships:
“doesn’t have any friendships…needs social communication aside from that kind of input … the group is good as it gets him used to it.” (Jane, Occupational Therapist, School).
College participants reported that any immediate changes following the sensory integration groups were visible for the remainder of the day, although any carryover to the following day was uncertain.
All participants appeared to link increased time spent in the groups with increased participation in subsequent learning activities:
“When they come back [from the groups] they are much more settled…..it can be helping them to calm down and re-engage in the next sort of lesson or next part of the lesson” (Felicity, SLT)
Emma (Teaching Assistant, College) described how one learner’s participation levels changed following the groups. Initially they were ‘unsettled and difficult to manage’, but they became more ‘co-operative, focussed and communicative’. She felt that the groups ‘calmed’ and ‘settled’ this learner in preparation for the next academic lesson.
Different staff members worked with learners at different stages of the day and the occupational therapists, for example, had limited contact with learners following a group. As a result they mainly described behavioural changes during the groups. Difficulty evaluating outcomes was referred to by all college participants, who highlighted the difficulty gaining feedback from learners themselves, mainly due to their cognitive abilities. Nonetheless, indirect feedback could be sought from behaviour during and following the sensory integration groups:
“…he is happier on Wednesday afternoons…smilier… calmer…whereas normally he’s quite manic and very er pacing” (Emma, Teaching Assistant, College).
“…engaging for longer and able to participate for the whole session really” (Rachel, Occupational Therapist, College).
Sally (Occupational Therapist, College) acknowledged the challenge of evaluating the impact of the groups, raising the possibility that it could be participation in activity, rather than sensory integration per se, that resulted in behavioural changes. All participants saw the groups as part of wider therapeutic input:
“I don’t think it is all OT, I think it’s global, I think we play a part in it.” (Fiona. Occupational Therapist, College).
Accessing the subjective experiences of college and school staff working directly with learners allowed opportunity to explore subtle behavioural changes following sensory integration input, as encouraged by Watling and Deitz (2007). This has provided insight into the impact on participation within the educational context. The findings suggest that therapists and teachers working with individuals with learning disabilities, autism and other complex needs consider that occupational therapy groups based on sensory integrative principles can have a positive impact on the underlying abilities and participation of those attending. Measuring that impact is, however, perceived to be difficult and the degree to which improvement results from the sensory integration groups or other therapeutic input is uncertain. These findings resonate with similar studies, as will now be discussed.
For children with complex needs such as autism and learning disabilities, the process of interpreting the sensory demands of the environment can be disrupted, resulting in difficulties participating in key activity necessary for development such as learning, play and social interaction (Ayres, 2005, Schaaf and Nightlinger, 2007). The complexities of impaired sensory processing and resulting disruption to participation were described in detail by participants, who referred to sensory integrative problems leading to anxiety and challenging or self-injurious behaviour, reflecting other studies (Urwin and Ballinger, 2005, Schaaf et al., 2013). The most common reasons for referral to the sensory integration groups (motor planning, response regulation, challenging behaviour and ability to remain in and participate in teaching sessions) are all key areas in which these populations may experience difficulties. This supports the highlighted need for regular, intensive, individualised intervention (May-Benson and Koomar, 2010, Polatajko and Cantlin, 2010).
The findings in both studies suggest that participation in sensory integration groups is perceived to be beneficial in addressing several of these issues for children and young adults. Participants described changes in underlying capacities and behaviour leading to increased participation, in particular improved engagement in learning activities and self-help skills. This resonates with many of the studies conducted with children (for example Case-Smith and Bryan, 1999 and Smith Roley et al., 2009) which might suggest that those authors’ findings are equally applicable to young adults. Improved cognitive and motor planning skills have been suggested elsewhere to lead to increased engagement in learning activities and self-help skills (Ayres, 1972, Schaaf and Nightlinger, 2007) promoting academic learning, flexibility, social interaction and development of interests.
All school participants described learners appearing calmer following the sensory integration groups, suggesting that attendance had improved regulation of arousal levels and integration of vestibular, proprioceptive and tactile sensory systems. This supports the use of sensory integration-based interventions using equipment such as weights, swings and scooter boards to help promote the integration of these systems. In both settings, references were made to improved behaviour as a result of attending the groups. Although this has not been widely explored in the literature, perceived reductions in challenging behaviours have been found in other studies (Urwin and Ballinger, 2005, Watling and Deitz, 2007). Improved arousal regulation was perceived to promote engagement in subsequent activities, (as argued by Urwin and Ballinger, 2005 and Waitling and Deitz, 2007). Examples given by participants include leisure activities (listening to music and dance classes) and self-care activities (eating in the dining hall and exercise). Improved arousal regulation and the increased attention and focus observed in some participants following intervention fits with Ayres’ theory (2005), and adds to other evidence of the effectiveness of sensory integration in promoting children’s participation (Schaaf and Nightlinger, 2007, Watling and Deitz, 2007). Schaaf and Nightlinger (2007) reported improved attention in play and school activities alongside increased independence in self-care activities, following individual sensory integration-based interventions.
Participants highlighted how taking part in the sensory integration groups themselves was an opportunity for socialisation, development of skills such as turn taking and waiting, valuable for young people with complex needs such as autism and learning disabilities (Cosbey et al., 2010). These groups were perceived by participants as having become meaningful to some learners and changes in behaviour, and levels of participation within the sensory integration groups themselves were seen as important in the context of these young people with complex needs.
As well as visible changes within the groups there were suggestions of longer-lasting benefits, such as subtler behavioural changes over longer periods. This included enhanced confidence and learners developing a sense of self identity, reflected also in other studies (Urwin and Ballinger, 2005). This all suggests potential for the benefits of sensory integration groups to be transferred beyond the immediate setting to further enhance the quality of life of young people with learning disabilities. Lasting impact following the groups was, however, difficult for some participants to judge, as not all of them worked with learners immediately following sensory integration groups
Similar to other research in this field, this is a small scale study. The findings represent the perceptions of a small number of participants, discussing learners who had participated in sensory integration groups in two educational settings. As such, the potential for generalisation is limited, though detailed description allows transferability by the reader.
Key participants in the studies, the occupational therapists, were involved in setting up and leading the groups. They were in a position to have insight into the immediate impact and effectiveness of the groups, though the possibility of them wishing to portray them in a positive light needs to be considered. They arguably had a vested interest in seeing the outcomes of the sensory integration groups as the cause of perceived changes in behaviour either immediate or longer term following the intervention
Sensory integrative problems do not exist in isolation and the nature of learners’ additional cognitive and behavioural issues were only partially described by participants. In both settings the young people received a wide range of therapeutic, behavioural, and educational interventions and participants raised the possibility of these, or the act of participation in a group activity (rather than specifically a sensory integration group) also contributing to changes in behaviour.
Sensory integration techniques are commonly used by occupational therapists with young people and adults with autism and sensory and learning disabilities but there is a paucity of supporting evidence for this. This qualitative research suggests that group sessions involving sensory integration techniques are perceived to have a positive effect on the abilities and participation of children and young adults with learning disabilities and other complex needs in educational settings. It has provided rich descriptions of materials and activities used, specific changes in participation, perceived long- and (in particular) short-term impact of the sensory integration groups, contributing to calls for a stronger evidence base and a better understanding of the relationship between sensory integration therapy and the everyday lives of children and families (Cohn, 2001, Arbesman and Lieberman, 2010, Polatajko and Cantlin, 2010).
The findings are of relevance to occupational therapists and others working with young people with complex needs in special educational and other settings such as community, inpatient and residential settings. The findings add to evidence from other studies supporting the use of sensory integrative activities to increase independence and participation, particularly in learning activities (Urwin and Ballinger, 2005, Watling and Deitz, 2007). In particular, they suggest variables that may have the potential to be measured in future research, which could triangulate perceptions of the impact on performance capacity and participation, using observation or other methods of evaluating such changes.
Arbesman, M. and Lieberman, D. (2010). Methodology for the systematic reviews of occupational therapy for children and adolescents with difficulty processing and integrating sensory information. American Journal of Occupational Therapy. 64(3):368-374.
Ayres, A. J (2005).Sensory Integration and the Child 25th Anniversary Edition. CA: Western Psychological Services.4-14.
Ayres, A. J. (1972).Sensory integration and learning disorders. Los Angeles: Western Psychological Services.
Banner, D. (2010). Qualitative interviewing: preparation for practice. Canadian Journal of Cardiovascular Nursing. 20(3): 27-30.
Braun, V. and Clark, V. (2013). Using thematic analysis in psychology. Qualitative Research in Psychology. 3 (2): 77-101.
Bundy, A., Lane, S., Murray, E. eds (2002). Sensory Integration: Theory and Intervention. 2nd ed. Philadelphia: F A Davis Co.
Case-Smith, J. and Bryan, T. (1999). The effects of occupational therapy with sensory integration emphasis on preschool-age children with autism. American Journal of Occupational Therapy. 53(5): 489-497.
Cohn, E. S. (2001). Parent perspectives of occupational therapy using a sensory integration approach. American Journal of Occupational Therapy. 55: 285–294.
College of Occupational Therapists (2015). Practice briefing: sensory integration. London: COT.
College of Occupational Therapists (2012). Research and development strategic vision and action plan for occupational therapists working with people with learning disabilities. London: COT.
Cosbey, J., Johnston, S. and Dunn, M.L. (2010). Sensory processing disorders and social participation. American Journal of Occupational Therapy. 64(3): 462-473.
Creswell, J.W. (2013). Qualitative inquiry & research design: choosing among five approaches. Los Angeles: SAGE Publications Inc.
Cribbin, V. and Lynch, H. (2014). Using sensory integration to understand and intervene with children who have sensory needs. Cork: University College for Sensory Integration Network.
Department of Health (2001) Valuing People. London: Department of Health
Department of Health (2011). Improving Outcomes in Mental Health: our shared objectives. In No Health Without Mental Health for people of all ages. London: DH
Doig, E., Fleming J., Kuipers P. (2008). Achieving optimal functional outcomes in community-based rehabilitation following acquired brain injury: a qualitative
investigation of therapists’ perspectives. British Journal of Occupational Therapy. 71(9): 360-370.
Lang, R., O’Reily, M., Healy, O., Rispoli, M.,Lyndon, H.,Streusand, W.,David, T.,Kang, S.,Sigafood, J.,Lancioni, G., Diddo, R., Giesbers, S. (2012).Sensory Integration Therapy for Autism Spectrum Disorders: A Systematic Review. Research in Autism Spectrum Disorders. (6): 1004-1018.
May-Benson, T., Koomar, J. (2010). Systematic review of the research evidence examining the effectiveness of interventions using a sensory integrative approach for children. American Journal of Occupational Therapy. 64(3), 403-414.
Miller,L.J., Coll,J.R. and Schoen, S.A. (2007). A randomized control pilot study of the effectiveness of occupational therapy for children with sensory modulation disorder. American Journal of Occupational Therapy. 61, 228-238.
Polatajko, H and Cantlin, N (2010). Exploring the effectiveness of occupational therapy interventions, other than the sensory integration approach, with children and adolescents experiencing difficulty processing and integrating sensory information. American Journal of Occupational Therapy. 64(3), 415-429.?
Polatajko, H. J., Law, M., Miller, J., Schaffer, R., & Macnab, J. (1991). The effect of a sensory integration program on academic achievement, motor performance, and self-esteem in children identified as learning disabled: Results of a clinical trial. OTJR: Occupation, Participation and Health. 11, 155–176.
Roberts, J.E., King-Thomas, L. and Boccia, M.L. (2007). Behavioral indexes of the efficacy of Sensory Integration Therapy. American Journal of Occupational Therapy, 61: 555-562.
Schaaf, R and Nightlinger, K (2007).Occupational Therapy using a sensory integrative approach: a case study of effectiveness. American Journal of Occupational Therapy. 61(2): 239-246.
Smith Roley, S., Bissell, J. and Clark, G.F. (2009). Providing occupational therapy using sensory integration theory and methods in school-based practice. American Journal of Occupational Therapy. 63(6): 823-842.
Stonefelt, L.L. and Stein, F. (1998). Sensory integrative techniques applied to children with learning disabilities: an outcome study. Occupational Therapy International. 5(4): 252-272.
Urwin, R. and Ballinger, C. (2005). The effectiveness of sensory integration therapy to improve functional behaviour in adults with learning disabilities: five single-case experimental designs, British Journal of Occupational Therapy. 68(2): 56-66.
Watling, R. L. and Deitz, J. (2007). Immediate effect of Ayres’s sensory integration–based occupational therapy intervention on children with autism spectrum disorders. American Journal of Occupational Therapy. 61: 574–583.