Introduction
Following a Public Inquiry led by Robert Francis into the reasons why poor care at the Mid Staffordshire NHS Foundation Trust was not challenged by a wide range of National Health Service (NHS) regulatory bodies between 2005 and 2009, the Department of Health (DoH) has committed to the implementation of more than 200 recommendations for change in both primary and secondary care. Planned developments range from increasing the powers of government-sponsored health and social care regulator the Care Quality Commission, to promoting cultural change throughout the NHS (DoH, 2014). The stated aim of these changes is to protect patients from unacceptable and unsafe care in the future (Francis, 2013; DoH, 2014).
This review was written as background for research on ways in which the recommendations of the Francis Report may relate to the education of healthcare professionals. Its objective is to to identify the key themes underlying the 290 recommendations of the Francis Report, and to consider these themes in the context of recent NHS policy for England. Archived documents are used to trace the course of policy developments, from the New Labour reforms of the early noughties, through to the coalition governement’s Health and Social Care Act 2012, and the publication of the Report of the Mid Staffordshire NHS Foundation Trust Public Inquiry in 2013.
The relevance of key DoH policies to events occuring at the Mid Staffordshire NHS Trust will be explored, and reasons examined for the widely expressed view (Moore, 2013) that, in the current political climate, there is a serious risk that the recommendations of Francis will be implemented only where they coincide with pre-existing DoH policies.
Preliminary search of the literature relating to the Francis Report and the education of healthcare professionals
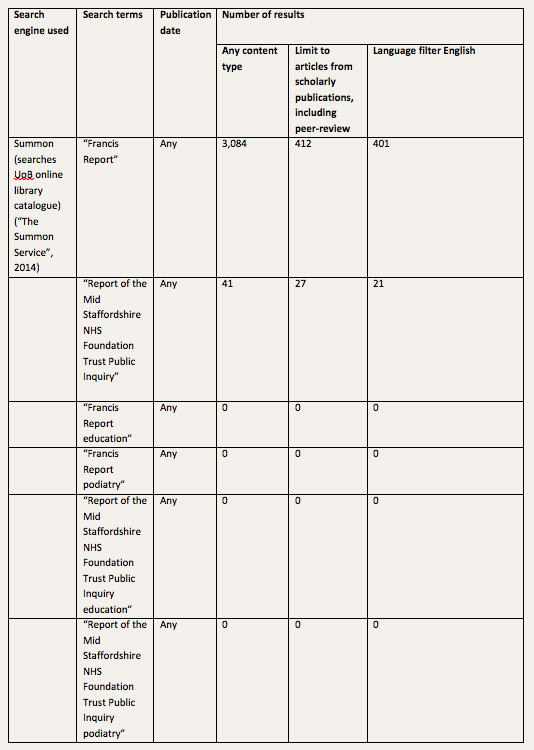
A preliminary search of the literature identified no published research relating to ways in which the Francis recommendations may be applied, either to the education and continuing professional development (CPD) of healthcare professionals in general, or of podiatrists in particular. The University of Brighton online library catalogue was searched using the terms: “Francis Report”; “Report of the Mid Staffordshire NHS Foundation Trust Public Inquiry”; “Francis Report education”; “Francis Report podiatry”; “Report of the Mid Staffordshire NHS Foundation Trust Public Inquiry education”; and “Report of the Mid Staffordshire NHS Foundation Trust Public Inquiry podiatry”. A summary of search strategy, search terms and number of results returned is presented in Table 1.
Table 1. Preliminary search of the literature relating to the Francis Report and the education of healthcare
professionals: search strategy, search terms and number of results returned
Review
The Report of the Mid Staffordshire NHS Foundation Trust Public Inquiry: a socio-historical context
The process of mapping recent NHS policy developments as a context for the recommendations of the Francis Report (Francis, 2013) began with Not the Francis Report: a National Voices Report on How to Ensure Safety & Quality (National Voices, 2012). (See also, Discussion, below.)
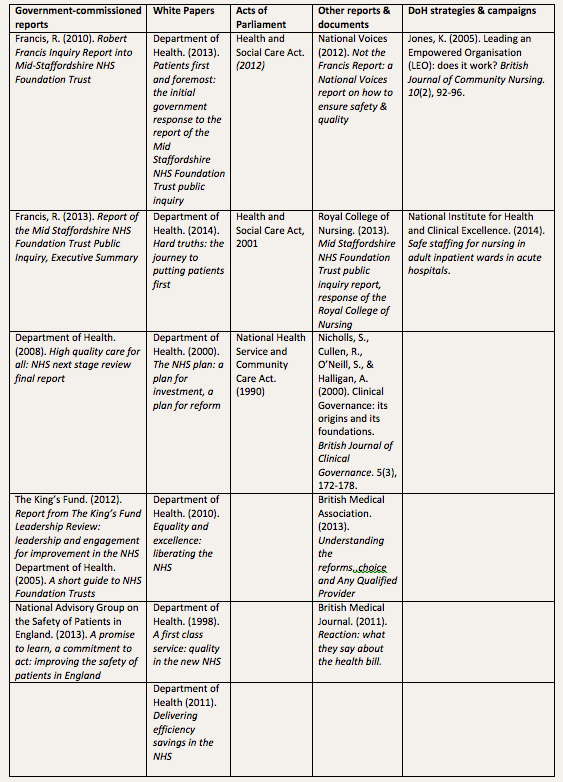
21 key documents were reviewed: five government-commissioned reports; six White Papers; four Acts of Parliament; five reports not commissioned by the government, and two pieces of comment and analysis. A classification of the literature reviewed is presented in Results, Table 2 (below).
Mechanism for review of archive material
Data extracted from each document
- Title
- Author
- Author background
- Date
- Publisher
- Summary
Data analysis is descriptive
Results
A classification of the literature reviewed is presented in Table 2.
Table 2. Classification of the literature reviewed
Discussion
Underpinning the 290 recommendations of his Report, Robert Francis identifies six core themes: culture; compassionate care; leadership; standards; information; and openness, transparency & candour (DoH, 2014, p.9).
With the purpose of developing these themes, the initial government response to the Francis Report (DoH, 2013) included the commissioning of a number of further reports, including one from Professor Don Berwick (National Advisory Group on the Safety of Patients in England, 2013) asking for ways to make “zero harm a reality in our NHS”. A summary of Berwick’s recommendations (see Figure 3, below) can be read as a summary of the themes underpinning the recommendations of the Francis Report.
Figure 3.Key themes underpinning the recommendations of the Report of the Mid Staffordshire NHS Foundation Trust Public Inquiry (aka the Francis Report)
(Francis, 2013; National Advisory Group on the Safety of Patients in England, 2013)

Concepts of “patient-centred” care and “putting patients first”
As reflected in its title, Hard truths: the journey to putting patients first, the DoH response to the Francis Report places the allied concepts of “patient-centred” care and “putting patients first” at the centre of its stated ambitions for NHS change (DoH, 2014). “Patient-centred” care is characterised as the experience of being treated as a “person rather than a number” (DoH, 2014, p.38), while the related concept of “putting patients first” is defined as “placing the quality of patient care, especially patient safety, above all other aims” (National Advisory Group on the Safety of Patients in England, 2013, p.36). Both these ideas can be seen to reflect Minister for Health, Lord Ara Darzi’s 2008 definition of high-quality care, as care that is “clinically effective, safe and personal” (DoH, 2008, p.8).
Cultural change through lifelong learning
The key strategy proposed by Francis, both for the delivery of patient-centred care and also for the implementation of his recommendations generally, is the promotion of cultural change throughout the healthcare system (Francis, 2013) (see also Figure 1, below). Francis (2013) and many others, including the DoH (2014), the King’s Fund (2012), and the National Advisory Group on the Safety of Patients in England (2013), identify the professional training and CPD of clinicians and health service managers as a key tool for the achievement of this cultural change.
But what does it all add up to?
In Not the Francis Report: a National Voices Report on How to Ensure Safety & Quality (2012), Don Redding, director of the coalition of health and social care charities, National Voices, argues that there was no need for a report from Francis and his team, that “ample evidence and consensus already exists” (p.2) to support reforms that will improve the quality and safety of health and social care. Redding (2012) argues that the themes identified by both Berwick and Francis (above) are not new. He suggests, instead, that attempts to address these themes form a thread that weaves its way through the history of NHS policy. Exploring this idea, these themes will be traced through three recent NHS White Papers (3.3.1 to 3.3.3, below) and compared against the recommendations of the Francis Report (2013).
The NHS Plan: a plan for investment, a plan for reform (DoH, 2000)
In July 2000, Tony Blair’s Labour government published the NHS Plan: a plan for investment, a plan for reform. This White Paper is built on earlier ground-breaking policy documents including A first class service: quality in the new NHS (DoH, 1998) and Clinical governance: its origins and foundations (Nicholls, Cullen, O’Neill, & Halligan, 2000). Like Francis (2013) and others (DoH, 2014, National Advisory Group on the Safety of Patients in England, 2013), the authors of both these documents emphasise the need for system-wide cultural change that includes reflective learning, staff development and patient-centred care based on partnership between patients and professionals.
Through the first half of the noughties, one notable and generally well-reviewed strategy for the achievement of the desired cultural change was the delivery, to 40,000 NHS staff, of a three-day management skills course known as Leading an Empowered Organisation, or LEO (Jones, 2005).
Setting out plans for a “reformed and patient-centred NHS”, the NHS Plan: a plan for investment, a plan for reform became law as the Health and Social Care Act, 2001. A key policy strategy included the establishment of Primary Care Trusts (PCTs), designed to improve the integration of health and social care by commissioning both of these services together. Major investment in clinical staff aimed to reduce long waiting times for treatment and to abolish the ‘postcode lottery’ in standards of care (DoH, 2008).
Staffing levels
It is noted that, as at the turn of the century, NHS staffing levels remain a contentious issue today, with a policy of inadequate staffing identified as a significant contributory factor to failures in care at Stafford Hospital (Francis, 2013).
As recommended by Francis, all NHS Trusts are now required to publish monthly, ward-by-ward nursing and midwifery staff numbers (DoH, 2014). In addition, the National Institute for Care Excellence (NICE) has published guidelines for staffing levels in adult inpatient wards in England (NICE, 2014). In contrast to the generous financial provisions of the 2001 Health and Social Care Act however, present-day requirements for major financial savings (DoH, 2011) make it unclear how far these staffing guidelines are likely to be implemented in practice.
The development of NHS Foundation Trusts
With direct relevance to the events at Stafford Hospital between 2005 and 2009, under the Health and Social Care Act 2001 high-performing NHS Hospital Trusts were granted ‘Foundation Trust’ status and a degree of independence from DoH control (DoH, 2005). The aim of Foundation Trust status is identified as allowing health service managers freedom from centralised decision making, thereby increasing patient choice through the delivery of health services that are responsive to local needs (DoH, 2005).
Despite the disastrous standards of care reported by Robert Francis within the Mid Staffordshire NHS Foundation Trust (Francis, 2010), the Health and Socal Care Act 2012 states that all NHS Hospital Trusts should aim to become NHS Foundation Trusts by April 2014.
Under the Health and Social Care Act 2012 and in line with the recommendations of the Francis Report, the DoH has recently increased the powers of the independent regulator of Foundation Trusts, Monitor (DoH, 2012; DoH, 2014). This development is opposed by influential commentators including Don Redding (National Voices, 2012), and Dr Hamish Meldrum (British Medical Journal, 2011), who believe that while regulatory bodies such as Monitor and the Care Quality Commission need to work better together, increasing their regulatory powers is likely to have a negative effect on patient care.
High quality care for all: NHS next stage review final report (DoH, 2008)
Aiming to reflect the views of 60,000 NHS staff and patients, and led by surgeon and Minister for Health, Lord Ara Darzi, this document presents the Labour government’s 10-year plan for the NHS.
Building on the Health and Social Care Act 2001, the key policy aim of this White Paper is identified as improving the quality of NHS healthcare, with ‘quality’ defined as care that is clinically effective, personal and safe. As in the Health and Social Care Act, 2001, this definition of high-quality care echoes the concepts of “patient-centred” care and “putting the patient first” that are identified by Robert Francis (2013) as the foundation stone of his recommendations for change.
Evidence-based practice
Building on documents such as Cullen, O’Neill & Halligan’s Clinical governance: its origins and foundations (2000), Darzi’s 10-year plan identifies the continued development of NICE guidelines and NHS Evidence as an important strategy for the delivery of high-quality care through evidence-based clincal practice. This is a strategy that continues to play an important role in the delivery of NHS healthcare, with Equality and excellence: liberating the NHS (DoH 2010) promising a “relentless focus on clinical outcomes” p.4.
Valuing NHS staff
Like Francis, Darzi identifies staff wellbeing and CPD as key to the delivery of high-quality care. Pledges on these issues are laid down in the first NHS Consitution, developed as part of this White Paper (DoH, 2008, p.77). Strategies for enhancing staff wellbeing include investment in preceptorships and apprenticeships, and a commitment to ensuring opportunities for CPD. By specifically rejecting the setting of any further national targets, Darzi acknowledges, and aims to reduce, the heavy administrative burden on clinical staff.
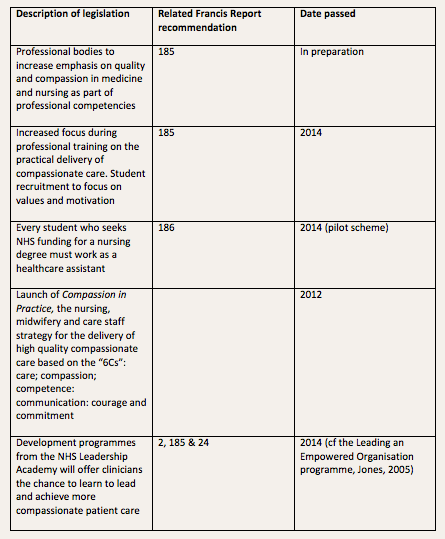
This commitment to reducing target setting is reiterated both in Equality and excellence: liberating the NHS (DoH 2010) and in the DoH response to the Francis Report (2014). In addition, like Darzi, the DoH (2014) identifies CPD as a key area for development within the health service. Based on strong recommendations from both Francis (2013) and the National Advisory Group on the Safety of Patients in England (2013), The DoH (2014) states that “Education and training should be a running theme throughout a healthcare practitioner’s career” (DoH, 2014, p.93). Developing this theme the government response to Francis continues that, as supportive management that facilitates staff engagement is shown to deliver better patient outcomes (King’s Fund, 2012), it must be “implemented with the rigour of a new drug” (DoH, 2014, p.91). To date, these ideas are yet to be translated into significant policy. A summary of proposed or actual changes to healthcare education legislation in response to the recommendations of the Francis Report is presented in Table 3.
Table 3. Summary of proposed or actual changes to healthcare education legislation in response to the recommendations of the Francis Report
Empowering clinicians and increasing patient choice
With the aim of empowering clinical staff to “set the direction of the services they deliver” (DoH, 2008, p.64), Darzi’s 2008 White Paper gave high-performing GP practices the freedom to offer previously hospital-based services, such as diagnostic imaging, in a primary care setting. Expanding on this theme, GPs were enpowered to buy services not only from the NHS, but also from the private and charity sectors, so that all patients referred for hospital treatment were now able to choose from several NHS and private sector providers (British Medical Association, 2013). Under the Health and Social Care Act 2010 this idea has been developed further, to become the controversial Any Qualified Provider scheme, whereby services are delivered by any qualified private provider on a payment-by-patient basis (DoH, 2010).
Equality and excellence: liberating the NHS (DoH, 2010)
Published only two years after Darzi’s 10-year plan, Equality and excellence: liberating the NHS sets out the new coalition government’s vision for the NHS.
Like Darzi’s 10-year plan, the stated aims of this White Paper include putting patients first and improving healthcare outcomes, with the expansion of patient choice identified as a key strategy for the achievement of these goals. A more controversial proposition is the idea that increased competition, in the form of the Any Qualified Provider scheme, will bring about improvements in the performance of healthcare providers. Key policies include abolishing the PCTs established by the New Labour government in 2001, and delegating their health-care-commissioning role to GPs overseen by an independent NHS Commissioning Board. In contrast to earlier policies designed to facilitate closer integration of health and social care services (DoH, 2001), social care is to be commissioned separately, by the Local Authority.
The policies of this White Paper were formally opposed by many professional bodies, including the British Medical Association, the Royal College of General Practitioners, the Royal College of Nursing and the Allied Health Professions Federation (Rogers, 2012). Two issues identified as key causes for concern are, firstly, that the fast pace of policy change poses an excessive risk to patient safety; and secondly, that by forcing GP commisioners to offer NHS contracts to private providers, the AQP scheme risks destabiising local health economies and making collaberative work in multi-disciplinary teams more difficult.
In a demonstration of misalignment between stated DoH aims and likely results of DoH policy, Hard Truths: the journey to putting patients first (DoH, 2014) makes frequent reference to the importance of supporting NHS staff to work effectively in multi-disciplinary teams, a well-evidenced strategy for the delivery of safer, more effective healthcare. Clinicians, including Dr Peter Carter of the Royal College of Nursing, and Dr Hamish Meldrum of the British Medical Association, argue that by fragmenting integrated care pathways, the AQP scheme will make services less efficient and put patient safety at risk (British Medical Journal, 2011). in March 2012, Equality and excellence: liberating the NHS was passed into law as the Health and Social Care Act, 2012.
Echoing the concerns of the professional bodies, Francis comments that insufficient risk assessment appears to have been undertaken by the DoH with regard to the implementation of system-wide change (2013 p.63). He goes on to note his impression that clinician advisors to the DoH are not at the heart of policy making on a number of issues, including the Foundation Trust agenda. He concludes that this lack of clinician involvement in policy making is likely to have negative implications for patient safety throughout the NHS.
Conclusions
Aiming to consider The Report of the Mid Staffordshire NHS Foundation Trust Public Inquiry in a socio-historical context, this review begins by identifying the key message of the Francis Report as an urgent need for widespread cultural change throughout the NHS. The overarching goal of this cultural change is to ensure that patients are protected from inadequate and unsafe care such as that provided at Stafford Hospital between 2005 and 2009.
Comparing the key themes underlying the recommendations of the Francis Report with the policy aims and strategies of three recent DoH White Papers, the hypothesis is supported that the themes identified by Francis are not new, but rather form a thread that weaves its way through recent NHS policy. A number of recurring themes are identified, including the key role of CPD in the delivery of high-quality healthcare, the need for partnership between patients and clinicians, and policy maker ambitions to increase patient choice.
Reflecting the concerns expressed by many professional bodies, Francis highlights the risk that, by demanding rapid organisational change (DoH, 2010) allied to tight financial control (DoH, 2011) , current DoH policies may compromise the ability of the NHS to deliver the identified goal of safe, patient-centred care. Healthcare commentators argue that, against the current poliitical background, many of the recommendations of the Francis Report may be more wishful thinking than a practical blueprint for change (Moore, 2013).
Nancy Jones, Podiatrist and Dr. Christopher Morriss-Roberts, Senior Lecturer, School of Health Sciences
References
British Medical Association. (2013). Understanding the reforms..choice and Any Qualified Provider. Retrieved March 3, 2014, from http://www.bma.org.uk/-/media/…/understandnhsreforms_choice_aqp_apr2013.pdf
British Medical Journal. (2011). Reaction: what they say about the health billl. Retrieved 15 July 2014 from http://www.bmj.com/content/342/bmj.d413.full
Department of Health. (2000). The NHS plan: a plan for investment, a plan for reform. (Cm 4818-1). London: HMSO. Retrieved 15 January 2014 from http://pns.dgs.pt/files/2010/03/pnsuk1.pdf
Department of Health (2005). A short guide to NHS Foundation Trusts. London: HMSO. Retrieved 15 July 2014 from http://webarchive.nationalarchives.gov.uk/20130107105354/
Department of Health. (2008). High quality care for all: NHS next stage review final report. (CM 7432). London: HMSO. Retrieved 15 January 2014 from http://www.official-documents.gov.uk/document/cm74/7432/7432.pdf
Department of Health. (2010). Equality and excellence: liberating the NHS (CM 7881). London: HMSO. Retrieved 15 January 2014 from https://www.gov.uk/government/uploads/system/uploads/attachment_data/file/213823/dh_117794.pdf
Department of Health (2011). Delivering efficiency savings in the NHS. Retrieved May 15, 2014, from www.nao.org.uk/wpcontent/uploads/2011/12/NAO_briefing_Delivering_efficiency_savings_NHS.pdf
Department of Health. (2013a). Patients first and foremost: the initial government response to the report of the Mid Staffordshire NHS Foundation Trust public inquiry. London: HMSO. Retrieved 15 January 2014 from https://www.gov.uk/government/uploads/system/uploads/attachment_data/file/170701/Patients_First_and_Foremost.pdf
Department of Health. (2014). Hard truths: the journey to putting patients first. London: HMSO. Retrieved 15 January 2014 from https://www.gov.uk/government/uploads/system/uploads/attachment_data/file/270368/34658_Cm_8777_Vol_1_accessible.pdf
Francis, R. (2010). Robert Francis Inquiry Report into Mid-Staffordshire NHS Foundation Trust. London: HMSO. Retrieved 1 December 2013 from www. nationalarchives.gov.uk
Francis, R. (2013). Report of the Mid Staffordshire NHS Foundation Trust Public Inquiry, Executive Summary London: HMSO. Retrieved 1 December 2013 from www.official-documents.gov.uk
The Guardian. (2012). Health and social care bill: who’s against (and for) it? Retrieved January 21, 2014, from http://www.theguardian.com/news/datablog/2012/mar/19/health-social-care-bill-visualised#data
Health and Social Care Act. (2001). London: HMSO. Retrieved 15 January 2014 from http://www.legislation.gov.uk/ukpga/2001/15/contents
Health and Social Care Act. (2012). London: HMSO. Retrieved 15 January 2014 from http://www.legislation.gov.uk/ukpga/2012/7/resources
Jones, K. (2005). Leading an Empowered Organisation (LEO): does it work? British Journal of Community Nursing. 10(2), 92-96.
The King’s Fund. (2012). Report from The King’s Fund Leadership Review: leadership and engagement for improvement in the NHS. Downloaded 15 January 2014 from http://www.kingsfund.org.uk/sites/files/kf/field/field_publication_file/leadership-for-engagement-improvement-nhs-final-review2012.pdf
Moore, A. Mixed reviews for Francis’s epic. The Health Service Journal 2013; 123: 20-23.
National Advisory Group on the Safety of Patients in England. (2013). A promise to learn, a commitment to act: improving the safety of patients in England. London: HMSO. Retrieved 1 December 2013 from https://www.gov.uk
National Health Service and Community Care Act. (1990). London: HMSO. Retrieved January 15, 2014, from http://www.legislation.gov.uk/ukpga/1990/19/contents
National Institute for Health and Clinical Excellence. (2014). Safe staffing for nursing in adult inpatient wards in acute hospitals. Staffing guideline 1. http://www.nice.org.uk/Guidance/sg1
National Voices (2012). Not the Francis Report: a National Voices report on how to ensure safety & quality. Retrieved 15 January 2014 from http://www.nationalvoices.org.uk/sites/www.nationalvoices.org.uk/files/not_the_francis_report_final.pdf
Royal College of Nursing. (2013). Mid Staffordshire NHS Foundation Trust public inquiry report, response of the Royal College of Nursing. London: Royal College of Nursing. Retrieved 1 December 2013 from http://www.rcn.org.uk








