Introduction
The word ‘Humour’ originates from the Latin for ‘fluid’ (Buxman 2008). Historically it was believed that the body contained four ‘humours’ (Blood, Phlegm, Yellow Bile and Black Bile), which governed a person’s health (Scott 2007). Today, though humour is considered ‘the quality of being funny’ (Collins English Dictionary 2011) there is no universally accepted definition (Buxman 2008; Moran 1990). Humour has a multidimensional value in healthcare (Beck 1997, 346); to help calm patients (Beck 1997), as a stress coping strategy (Mildenhall 2012), educational tool (Baid and Lambert 2010), and for group cohesion (Watson 2011).
The question of what affect different types of humour and different humour styles might have upon stress coping strategies is a significant one (Dyck and Holtzman 2013); especially for healthcare (Moran and Massam 1997). The aim of this literature review is therefore to analyse what is currently known in this area, highlighting aspects relevant to paramedic practice and possibilities for future research.
Methodology
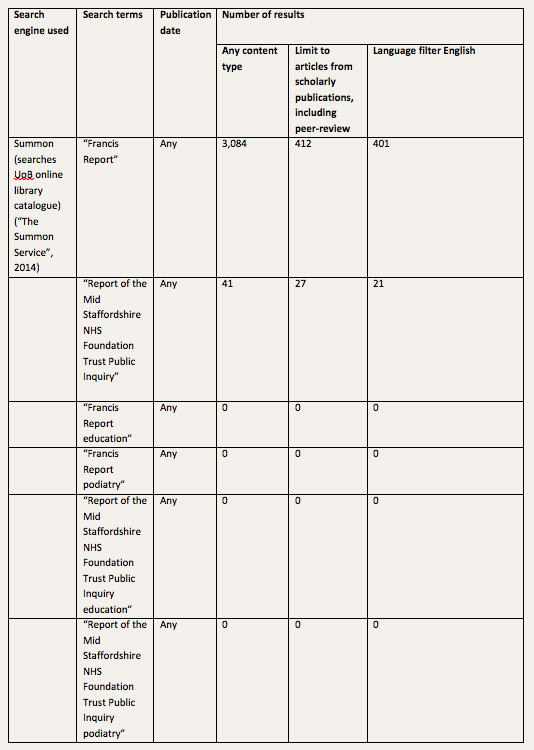
In order to achieve the aim of the study a systemic literature review was conducted. Initial searches of the Cumulative Index to Nursing and Allied Health Literature (CINAHL), PsycINFO, NHS Evidence, PubMed, ScienceDirect and Google Scholar databases using the keywords: burnout’ AND ‘paramedic’ OR ’emergency medical personnel’ OR ‘EMT’ OR ‘prehospital’ OR ‘pre-hospital‘, ‘resilience’ AND ‘paramedic’ OR ’emergency medical personnel’ OR ‘EMT’ OR ‘prehospital’ OR ‘pre-hospital‘, ‘humour’/ ‘humor’ AND ‘paramedic’ OR ’emergency medical personnel’ OR ‘EMT’ OR ‘prehospital’ OR ‘pre-hospital‘. The Boolean operators AND and OR were incorporated to combine search terms and focus results in the relevant area under consideration (Hart 2005). American/English spelling adaptations were included to locate all relevant literature (Moule and Goodman 2009). Searches yielded a significant number of studies but not all were available in full text. Those giving only abstracts were examined to see if they had noteworthy relevance; where found to, alternative avenues were investigated to acquire the full text. Some were obtained through online libraries via Google Scholar. Others, unavailable without payment, were excluded from the review. In order to conclude to the most suitable and narrow results the following inclusion and exclusion criteria were used:
Inclusion:
- Primary research: written by the person who developed the theory or conducted the original research (Polit and Beck 2006)
- Published in English
- Peer reviewed: research examined for bias or inappropriate subjectivity by the researcher’s peers or colleagues (Holloway and Wheeler 2010)
- Free to Access
Due to the relative infancy of research into burnout (Felton 1998) and the older study of humour use (McCreadie and Wiggins 2008) no year of publication boundaries were set; resulting in the discovery of research which significantly informed this review. Additionally, worldwide parameters were allowed to investigate whether use of humour might uncover research with cultural factors relevant to the diversity of healthcare workers in Britain. Though people from ethnic minorities made up only 2% of ambulance staff in 2005 (National Guidance Research Forum 2005) it could be argued that paramedics engage with many healthcare workers in and out of the NHS as part of their work, making this consideration initially relevant. However, as only a limited number of studies, of minimal relevance were uncovered this review concentrates on first world research.
Secondary sources ‘can provide rich data’ (Munhall 2007, 382), however, they are only used where primary research was unobtainable and then limited to discussion areas or additional reference support. This is because secondary sources are one author’s commentary upon another author’s primary research, which can raise concerns over interpretation or bias (Macnee and McCabe 2008).
The Journal of Paramedic Practice was manually searched (due to online inaccessibility) with one article uncovered, aiding discussion elements.
Data saturation ‘indicates that everything of importance to the agenda of a research project will emerge in the data and concepts obtained’ (Holloway and Wheeler 2010, 146). This point was considered reached after repeated searches revealed the same articles closest to the research question.
Qualitative research studies the meaning people give to phenomena (Parahoo 2006), whereas quantitative research investigates ‘phenomena lending itself to precise measurement’ (Polit and Beck 2010, 565). The framework of Lobiondo-Wood and Haber (2002) (appendix 2) for critiquing qualitative and quantitative research was used to critique the three main studies considered central to the research question. Additional research was identified using a snowballing technique – where references in one study lead to locating works by other authors (Polit and Beck 2010).
Results

Review of the research uncovered three main themes:
- Burnout: a condition experienced by paramedics
- Humour: a factor in stress relief and resilience
- Humour use by paramedics
Burnout: a condition experienced by paramedics
Originally used to describe the cessation of a jet engine, Felton (1998) additionally notes that in the 1970’s burnout was first applied to humans by psychologist Herbert Freudenberger. Freudenberger studied how healthcare personnel he worked with changed from being passionate about their job to becoming distant and apathetic; describing themselves as ‘burnt out’ (Ruysschaert 2009). Building on Freudenberger’s work, Maslach and Jackson (1981) published their research into the measurement of burnout, which became seminal for subsequent studies.
Burnout produces a combination of emotional exhaustion, de-personalisation, and reduced personal accomplishment (Maslach and Jackson 1981) being most frequently found among ‘human services professionals, particularly in healthcare’ (Felton 1998, 237). Chase (2014, 1) proposes that ‘no one burns out who wasn’t on fire to begin with’, suggesting burnout is peculiar to people with high expectations of themselves. Maslach and Leiter (2005) agree, proposing that idealists, perfectionists and those with a strong sense of purpose are most at risk. When ideals of relieving suffering, and expressing compassion, are thwarted by time or circumstance a sense of failure and inadequacy can lead to chronic stress and burnout (Chase 2014). The effect of burnout may include physical and emotional exhaustion, increased levels of anger, headache, insomnia, chronic hypertension, gastrointestinal complaints, immune dysfunction, infertility, sleep disorders (Felton 1998; Sophianopoulos, Williams & Archer 2012) as well as higher rates of alcoholism, drug abuse, increased smoking and caffeine intake and coronary heart disease (Frank and Ovens 2002).
Nirel et al (2008) identifies lack of administrative support, long hours, poor work / life balance, and poor salaries as causes of burnout in paramedics particularly. Sophianopoulos, Williams & Archer (2012) add shift work to this list. The impact of burnout upon paramedic’s families is also noted by Regehr (2005), significantly affecting the quality of interpersonal relationships. Increased levels of depression were noted by Griner (2013), with increased percentages of suicidal ideation acknowledged by Sterud et al (2008).
Much literature on burnout makes mention of Maslach and Jackson (1981), Griner (2013) noting burnout is usually measured in healthcare workers using Maslach’s Burnout Inventory (MBI) developed from this research. MBI is a self administered questionnaire which notes a range of responses to an individual’s feelings about their work (Kashka, Korczak & Broich 2011).
‘The Measurement of Experienced Burnout’ by Maslach and Jackson (1981) was first presented in the peer reviewed Journal of Occupational Behaviour, published by Wiley since 1980 (www.jstor.org). The authors acknowledge use of qualitative data drawn from other researchers, citing: Freudenberger (1974; 1975), Ryan (1971) and Wills (1978), as well as previous personal research (Maslach 1976), and collaborative work with Pines (1977), however no reference is made to any literature review being conducted. This is possibly due to the infancy of research into burnout at the time (Felton 1998) or that some researchers prefer a brief overview rather than comprehensive literature review to set their study in context (Polit and Beck 2004). Additionally, ethical considerations are not mentioned, though it is unlikely researchers would neglect the basic principles of safeguarding participant’s rights and ensuring their safety (Parahoo 2006). Furthermore, footnotes acknowledge the study was supported by a Bio-Medical Sciences grant, which is awarded only after submission of an application showing all research considerations have been covered (Polit and Beck 2004). Two sample groups were drawn from a range of human services occupations across America including: Physicians, Police, Psychiatrists, Nurses, Social Workers and Counselors. Qualitative data was gathered through semi-structured interviews – presenting a set of questions allowing for individual responses but leading to similar data from participants (Holloway and Wheeler 2010), and quantitative data through questionnaires – a means of collecting specific, measurable data (Holloway and Wheeler 2010). How participants were recruited is not recorded. An initial 47 item questionnaire concerning ‘feelings and attitudes about work’ was compiled with each statement rated on two dimensions: Frequency and Intensity. An answer range of 1-7 gave options between ‘never’, to ‘every day’. This questionnaire was initially administered to 605 people – being a large enough group to be representative of the whole 1025 member sample (Polit and Beck 2010).
Four factors were discovered from the data and titled: ‘Emotional Exhaustion, ‘De-personalisation‘, ‘Personal Accomplishment’ and ‘Involvement’. The fourth factor, though appearing consistently in the data was rejected as a subscale due to its eigenvalue ‘being inconsistent with reliability’ (Maslach and Jackson 1981, 104).
Since publication MBI has been tested by numerous researchers; Schaufeli and Enzmann (1998), cited by Glasberg, Eriksson & Norberg (2007) suggest 90% of empirical studies into burnout now use MBI, giving credence to its dependability. MBI has also been used in organisational settings other than healthcare, including a telecommunications company, pension company and insurance company (Gonzalez-Roma et al 2006) increasing confidence in the transferability of MJ findings.
MJ found that results due to age varied, with younger people scoring higher risk of burnout than older – this is potentially significant when compared to McAlister and McKinnon (2009) who found similar factors in their study of student and qualified paramedics in Australia. The suggestion of Gayton and Lovell (2012) that healthcare workers with longer service owe their resilience to an element of natural selection is also interesting to note in light of this. Married workers were found to have lower risk of burnout than single or divorced workers – possibly equated to the beneficial factor of greater social support noted by Gustafsson et al (2010) and Dyrbye et al (2010).
MJ conclude with the desire that MBI may lead to greater understanding of burnout, ‘influencing future job training, recruitment and design to alleviate the problem’ (Maslach and Jackson 1981, 112); its widespread adoption by researchers (as mentioned above) suggests some accomplishment of this.
Stress is a significant issue within the NHS with an estimated 30% of all staff sickness absence related to it (NHS Employers 2012). Paramedics are particularly susceptible to levels of stress that can lead to burnout (Regehr and Millar 2007) and like other human service workers they use diverse strategies to cope with it (Hawkins 2008). The following chapter examines one strategy, humour use, which has a particular relationship to the emergency services (Charman 2013).
Humour: a factor in stress relief and resilience
Defined as ‘the ability to rebound from adversity and overcome difficult circumstances in life’ (McAlister and McKinnon 2009, 372), resilience is identified by researchers as key in the avoidance of burnout (Gayton and Lovell 2012).
Resilience consists of different factors including level of social support and personality (Grafton, Gillespie & Henderson 2010). However, of all factors highlighted in the development of resilience, the use of ‘humour’ stands out as a common theme (Essex and Benz-Scott 2008; Felton 1998; Grafton, Gillespie & Henderson 2010; Griner 2013; Ruysschaert 2009; Strumpfer 2003).
A ‘complex phenomenon, incorporating cognitive, emotional, behavioural, physiological and social aspects’ (McCreadie and Wiggins 2009, 1079), studies have lead to three basic theories of humour types:
The Incongruity Theory: developed by Kant (1724-1804) notes the ‘punch line’ is different from that expected, – humour being derived from this mismatch (McCreadie and Wiggins 2008).
The Superiority Theory: developed by Plato (427-347) and Hobbes (1588-1679) suggests we laugh at the failings of others to feel better about ourselves (Feagai 2011).
The Relief Theory: developed by Freud (1856-1939) suggesting humour releases suppressed emotions (Hawkins 2008).
Though examples of all three can be found in resilience strategies, Freud’s theory is perhaps more significant as it aims to relieve anxiety and transform negative feelings (Buxman 2008). In ‘The Joke and its Relation to the Unconscious’ (Freud 2002), Freud suggests humour provides an acceptable form for raising taboo subjects, additionally offering a means for ridiculing and dis-empowering people’s fears. The idea of weakening a threat or fear through ridicule is one also attested to by Downe (1999) and Obrdlik (1942); McGhee (2013) suggesting this is due to the increased sense of control humour brings to stressful situations. Henman (2001) corroborates, having found humour fundamental to resilience amongst American prisoners of war in Vietnam and survivors of concentration camps. The significance of this is not lost when considering the stresses of emergency care.
Kuiper (2012), and Dean and Major (2008) found humour helped medical personnel distance themselves from stressful situations; Chinery (2007, 1) calling humour a ‘buffer’ against stress.
Several researchers note claims over the positive health effects of humour (McCreadie and Wiggins 2008) including: reduction of anxiety, increased pain tolerance, improved respiration (Buxman 2008), lowering of blood pressure (McCreadie and Wiggins 2008) and release of endorphins (Fabry 2011; Feagai 2011). However, the most cited case is that of Norman Cousins whose recovery from Ankylosing Spondylitis is often claimed due to humour use (Moran and Massam 1997).
In Anatomy of an Illness, Cousins states: ‘ten minutes of belly laughter had an anaesthetic effect giving me two hours of pain-free sleep.’ (Cousins 1979, 15) Rowe and Regehr (2010), and Mahony (2000) are not alone in challenging Cousins’ claims after subsequent research left them unproven.
On claims of stress reduction Moran and Massam (1997) cite Martin and Lefcourt (1983) who suggest sense of humour does not lead to decreased stress but rather that humorous people generate more humour to cope with stress. To the claim that humour increases pain tolerance, Weisenburg, Tepper & Swartzwald (1995) discovered humour had only a distracting effect, with similar results produced in sample participants watching horror films as humorous films (Weisenburg, Tepper & Swartzwald 1995, 210).
Mahony (2000) found no empirical support confirming laughter triggers endorphin release and suggests watching fish is as effective as humour at lowering blood pressure (Mahony 2000, 2). Mahony’s conclusion: ‘Humour trait is more beneficial than humour state’ (Mahony 2000, 2).
Research into humour use identifies four distinct humour styles revealing how people communicate with others, cope with stress, and build resilience (Dyck and Holtzman 2013): Affiliative Style: strengthening interpersonal relationships whilst maintaining positive self-esteem (Olson et al 2005), Self-Enhancing Style: Having a humorous outlook on life, boosting self-esteem and buffering against stress (Olson et al 2005), Aggressive Style: ‘put down’ humour / sarcasm and ridicule – often having a negative effect on interpersonal relationships (Kuiper 2012), Self-Defeating Style: being excessively critical or ridiculing of one’s self in an attempt to enhance relationships (Kuiper 2012).
For building resilience and coping with stress, affiliative and self enhancing humour are considered positive, whereas aggressive and self-defeating styles are considered negative (Hawkins 2008).
As well as acknowledging humour styles have positive and negative effects, Dyck and Holtzman (DH) questioned whether social support and gender might be factors which further influence the effect of these styles on well-being. Their quantitative method gathered a sample of 826 students, 65.3% Female, 74.3% Caucasian; with 88.7% between age 18-22. Participants were recruited through the psychology research pool at two Canadian universities. A ‘convenience sample’ – those most easily available (Polit and Beck 2010; Holloway and Wheeler 2010), this sample could be accused of bias (Polit and Beck 2004) as they were drawn from students interested in psychology research and therefore not truly representative of all university students. Data was gathered using online questionnaires, results being subjected to bivariate analysis – a means of quantitatively analysing two variables to determine the relationship between them (Babbie 2009). Analysis revealed:
Affiliative Humour was:
- The highest average score
- associated with lower levels of depressive symptoms
- associated with higher levels of life satisfaction
- associated with higher levels of perceived social support
Self-Enhancing Humour was:
- associated with lower levels of depressive symptoms
- associated with higher levels of life satisfaction
- associated with higher levels of perceived social support.
Aggressive Humour was:
- significantly higher in males than females
- not significantly associated with depressive symptoms, life satisfaction or levels of perceived social support.
Self-Defeating Humour was:
- The lowest average score
- associated with greater depressive symptoms
- associated with lower life satisfaction
- associated with lower levels of perceived social support.
DH suggest that affiliative and self-enhancing humour styles could be interpreted as more socially attractive and therefore act to increase a person’s social support, whereas aggressive and self-defeating styles could produce the opposite. However, they note a potential alternative explanation might be that social support has a controlling influence on humour styles and their affect on well-being. High social support might enhance the use of positive styles, and diminish the effect of negative styles; whilst lower social support may have the opposite effect.
The application of this study to the paramedic setting is interesting in that it suggests social support; gender and humour styles all have an effect on well-being and potential resilience levels. The Ambulance Service has been a traditionally ‘male’ dominated environment (Sterud et al 2008, Bennett et al 2004) with potential for steering humour towards aggressive styles, (possibly less beneficial for female staff). Levels of social support within the Ambulance Service have also been identified as significant in the area of burnout and resilience (Van de Ploeg and Kleber 2003). In the following chapter the issue of humour use by ambulance staff will be examined to consider its effect upon resilience to burnout.
Humour use by Paramedics
Rebuffing the idea that humour in healthcare is unprofessional, Dean and Major (2008) champion its value in aiding communication, managing emotion, team building and burnout avoidance. Furthermore, within emergency healthcare research a common theme is the use of ‘gallows humour’ (GH) for stress relief (Alexander and Klein 2001; Bennett 2003; Rosenberg 1991).
GH is often used at times of tragedy or death (Bennett 2003, 1259). Freud (2002) notes its use by individuals, but Obrdlik (1942), in a study of the Nazi invasion of Czechoslovakia, was one of the first to document its use by whole societies. Its use by groups in stressful work environments has since been acknowledged (Moran and Massam 1997).
Amongst many paramedics, GH is considered ‘the biggest coping mechanism we have’ (Villeneuve 2005, 8). Diminishing negative feelings by re-framing a horrific situation GH offers a defense in overpowering situations (Van-Wormer and Boes 1997); whilst ‘maintaining sanity under insane circumstances’ (Kuhlman 1988; cited in: Rowe and Regehr 2010, 449). Several researchers noted how paramedics use humour to develop their social support (Mildenhall 2012) and build group cohesion (Rowe and Regehr 2010).
A seminal, qualitative study into humour use by paramedics is Rosenberg (1991) ‘A qualitative investigation of the use of humor by emergency personnel as a strategy for coping with stress’, which compares humour use by experienced and student paramedics, noting the development and adaptation of humour through exposure to clinical experience and exploring how changes in humour use may be ‘an adaptive method for coping with stress’ (Rosenberg 1991, 197).
Longitudinal research – ‘examining changes in a group over time’ (Burns and Grove 2001, 251), was incorporated in studies of 10 (ultimately 9) student paramedics from a convenience sample of 37. Known as the ‘pre/post trained group’, they were firstly interviewed before training, and then interviewed again after training.
A second group of 10 ‘experienced’ paramedics with 1-7 years experience were additionally recruited and interviewed once only. Their results, compared with the first group, provided cross sectional data for the study. Cross sectional research gives data from ‘more than one group of subjects at various stages of development, simultaneously’ (Burns and Grove 2001, 252).
Though participant numbers were small, data saturation – where no new data is uncovered (Polit and Beck 2010) was highly probable as the groups were representative of the ‘student’ and ‘experienced’ populations. Data was gathered using a structured interview – ‘the same questions, in same order, with same response options’, (Polit and Beck 2004, 349), but with open ended questions – ‘giving freedom to respond in narrative fashion’ (Polit and Beck 2004, 349). Inductive analysis – taking specific facts to form general theory (Macnee and McCabe 2008), ‘without the restraints imposed by structured methodologies’ (Thomas 2003, 2), was employed to make maximum use of the data; enabling recurrent themes to be categorized and counted.
Charman (2013); Mildenhall (2012); and Rowe and Regehr (2010) acknowledge the same with regard to humour building group cohesion, teamwork and social support.
Context of EMS humour: The ‘experienced’ paramedics stated that ‘they could not share the humour they used at work with family or friends’ (Rosenberg 1991, 199). Bennett (2003) suggests that because humour exists within a certain culture, what is funny to some will not be to others. Those ‘outside’ the group (including family and friends) may be repelled by GH because they ‘cannot fully comprehend the reason for its origin’ (Rowe and Regehr 2010, 456).
Goffman (1959) presents the concept of regions of acceptable behaviour within society. Applied to humour use in healthcare, this proposes that emergency workers have ‘Frontstage’, ‘Backstage’ and ‘Offstage’ environments which moderate their behaviour (Williams 2013a). As part of the unwritten rule of GH use, it is only acceptable in the ‘Backstage’ environment of either the crew room or at an incident scene where no non-emergency personnel are present (Williams 2013a; Watson 2011; Mildenhall 2012). GH is never appropriate in the ‘Frontstage’ environment where patient relatives look to paramedics for support (McCarroll et al 1993), and is strongly discouraged in the ‘Offstage’ environment – at home or off duty when paramedics are with relatives and friends, as they are ’outside’ the circle for understanding the nature or origin of the humour (Rosenberg 1991).
Purpose of Humour use: All participants, except three from the pre/post group, stated they used humour as a coping strategy; with the entire experienced group rating it higher in importance as a strategy than any of the pre/post group. The students emphasised the tension relieving aspect of humour use after a bad day which is also acknowledged by Moran (1990), who considers humour more associated with reducing stress after an event rather than during (Moran 1990, 368). In contrast, the experienced group strongly emphasised the cognitive and emotional refocusing power of humour; as noted by Buxman (2008), Freud (2002) and Kotthoff (2006). Rosenberg therefore suggests humour use becomes a deepening or maturing stress defense for paramedics.
Discussion
 This review identified three main themes: ‘Burnout: a condition experienced by paramedics’, ‘Humour: a factor in stress relief and resilience’, and ‘Paramedic use of humour’.
This review identified three main themes: ‘Burnout: a condition experienced by paramedics’, ‘Humour: a factor in stress relief and resilience’, and ‘Paramedic use of humour’.
Chronic stress can lead to the three elements of burnout: emotional exhaustion, de-personalisation and diminished sense of accomplishment (Maslach and Jackson 1981). In healthcare this manifests as deterioration in the quality of care, high job turnover, absenteeism and increased health issues for those affected (Maslach and Jackson 1981). As paramedics are among those with the highest risk of burnout (Regehr and Millar 2007), this carries implications both individually and organisationally.
Implications for Paramedics
Maslach and Leiter (2005) and Chase (2014) suggest that a contributing factor in burnout of healthcare workers is the imbalance between the care they desire to give and the care they are able to give. For paramedics, shift work, pressure to meet targets, abuses of the service by some people, and poor work/life balance are elements which affect this (Mildenhall 2012; Nirel et al 2008; Regehr and Millar 2007; Sophianopoulos, Williams & Archer 2012).
Maslach and Leiter (2005) suggest that giving time to stress relieving pursuits such as sporting activities, hobbies and social relationships, enable individuals to defuse the stresses of work which lead to burnout. However, a consequence of shift work is that partners and friends may be at work themselves when paramedics are off duty, with repercussions for social relationships (Harrington 2001). In contrast, Sophianopoulos, Williams & Archer (2012) suggest that families of shift-workers often adapt to their situation, becoming more resilient. Further research in this area might reveal factors contributing to positive social adaptation, of benefit to paramedics.
Access to information on their patient’s outcome is a source of stress for some paramedics (Regehr and Millar 2007); the lack of such information leading to concerns over personal competency (Witmore 2013). Access to patient information is governed by the Data Protection Act (1998) making confidentiality a legal requirement in NHS employment contracts (Department of Health 2003). Legislation allowing paramedics access to information on their patient’s outcome would help reduce incident related stress and encourage reflection (Bishop 2013), potentially improving staff well-being and patient care (Okougha 2013).
Organizational implications
The Health and Safety at Work Act (1974) requires employers to do everything reasonably practicable to protect the health, safety and well-being of their employees, including minimising the risk of stress related illness. As an employer, ambulance Trusts are subject to this legislation. Occupational health departments aim to provide employees access to counseling services, post incident de-briefing opportunities and peer lead support groups (NHS Employers 2012). Additionally, the Boorman Review (Department of Health 2009) recommended the establishment of staff stress management initiatives to further address well-being issues.
The reluctance of paramedics to disclose the full stresses of their work to those in ‘off-stage’ environments means they rely on ‘backstage’ environments (crew-rooms) for relieving the pressure (Williams 2013a). With the introduction of ‘Make Ready’ (SECAmb 2010) where vehicles are re-stocked by contractors rather than crews; and the increased deployment of crews to stand by points, ‘backstage’ time could be significantly reduced. Though possibly beneficial for productivity this removes a potential stress relief outlet for paramedics (Mildenhall 2012). Research into the impact of these initiatives, as well as into ways ambulance services might be proactive in initiating positive approaches to staff at risk of burnout could contribute to a reduction in the strain placed upon services due to absenteeism.
Humour: a factor in stress relief and resilience
The potential of humour as a positive element within healthcare is acknowledged by numerous researchers (Dyck and Holtzman 2013; Rosenberg 1991; Scott 2007; Shepherd and Wild 2014; Watson 2011).
Of the three main Humour Theories (Incongruity; Superiority; Relief), Freud’s ‘Relief Theory’ has the strongest association to humour use by paramedics, suggesting humour can bring a culturally acceptable means of releasing suppressed emotion, dis-empowering a potential threat and re-framing unpleasant experiences into more emotionally and cognitively manageable ones (Buxman 2008; Downe 1999; Henman 2001; McGhee 2013). Mahony (2000, 2) considers ‘humour trait more beneficial than humour state’, a view given weight by studies into humour styles, whereby ‘affiliative’ and ‘self-enhancing’ styles have been found to have a positive influence upon resilience to stress and burnout; whereas ‘aggressive’ and ‘self-defeating’ styles can have a negative effect (Dyck and Holtzman 2013; Stieger et al 2011).
Implications for individuals and organizations
Dyck and Holtzman note how ‘aggressive’ humour styles are more common amongst men; whilst Mahony (2003); and Williams (2012), acknowledge that ambulance services are traditionally male dominated. Citing the Office of National Statistics, Williams (2012) highlights that in 2010 there were ‘approximately 13,000 male paramedics in the UK whilst the number of female paramedics was too small for a reliable estimate’ (Williams 2012, 370). However, figures for registered UK paramedics in November 2013 indicate 7667 female paramedics compared to 12451 male (HCPC 2013). These figures still reveal a predominantly male profession.
Though ‘aggressive humour style’ might not significantly affect male resilience levels, as Dyck and Holtzman (2013) hypothesise, the higher percentage of male paramedics may mean a dominant aggressive humour style exists culturally. As numbers of female paramedics rise the humour culture they encounter may, therefore, have implications for their resilience levels.
Humour use by Paramedics
Whilst humour use for calming patients and relieving stress has been noted, of particular interest is paramedic’s use of ‘gallows humour’ (GH).
Gallows Humour
Helping to re-frame stressful situations, making them more emotionally manageable (Van-Wormer and Bows 1996), GH is most often used in times of tragedy, oppression or death (Bennett 2003; Freud 2002; Moran and Massam 1997; Obrdlik 1942). Its use today being particularly prolific among emergency services personnel (Charman 2013; Mildenhall 2012; Watson 2011).
Rowe and Regehr (2010) point out that GH often appears in general society after a major disaster, suggesting GH offers a means of putting tragedy into perspective. The fact that GH use is prevalent among paramedics (who potentially encounter more traumatic situations than those employed outside emergency, medical or armed forces careers) is therefore understandable (Chase 2014).
Implications for Paramedics
The question of how humour use, particularly GH, relates to professionalism is an obvious one. The Health and Care Professions Council: Standards of conduct, performance and ethics (2012) highlights the expectation that registrants will deal respectfully towards service users, showing integrity, and the highest standards of personal conduct, whilst avoiding any action that would bring their profession into disrepute (HCPC 2012, 3). The potential for inappropriate humour use to breach these standards is strong. However, Rosenberg (1991); Rowe and Regehr (2010); and Williams (2012) indicate that tight boundaries for cultural humour use exist within ambulance services, where GH particularly is considered taboo outside specific environments, or with those outside the accepted group.
The concept of ‘Frontstage’, ‘Backstage’ and ‘Offstage’ environments (defined by whether any non-emergency personnel are present), has been suggested by Goffman (1959); Rosenberg (1991); Watson (2011) and Williams (2012). For paramedics, the ‘backstage’ environment, such as the station crew-room or ambulance vehicle cab, is considered the only one where GH is sanctioned. This self regulated cultural code of conduct would seem to act as a strong deterrent to breaches of professionalism, though cannot guarantee against them. The potential for GH between paramedics to be overheard by non-emergency personnel at the scene of a traumatic event is reasonably high and paramedics should be vigilant in guarding against it.
Implications for the future progression of the Paramedic profession
Literature considered in this review suggests the presence of a humour culture within the Ambulance Service that new recruits are socialised into (Rosenberg 1991). Furthermore, Essex and Benz-Scott (2008); McAlister and McKinnon (2009); Rosenberg (1991) and Villeneuve (2005), observe that recognition of the value of humour use as a coping strategy increases with clinical experience and years of service.
The role of socialisation in conforming new members of a group into cultural norms is a recognised phenomenon (Giddens and Sutton 2013). However, the question of whether socialisation into all aspects of ambulance humour culture is helpful or desirable within the modern Ambulance Service is potentially controversial. The benefits of appropriate humour use for relieving stress are attested to by many and not considered unprofessional (Dean and Major 2008). However, the more negative elements of humour culture such as overly aggressive humour styles and ‘put down’ humour, which Berk (2009) suggests is strongly associated with medical professions, may be unhelpful to some staff as the profession progresses.
Conclusion and Recommendations
This literature review has investigated the use of humour by paramedics as a factor in coping with stress and an element affecting resilience against burnout. Paramedic practice can be acutely stressful at times (Halpern et al 2012) though lower levels of chronic stress also exist within the role (Mildenhall 2012). The combination of this stress can lead to the emotional exhaustion, de-personalisation and loss of personal accomplishment that characterises burnout (Maslach and Jackson 1981).
Humour use has been identified as a factor in resilience and as a coping strategy against burnout among paramedics (Rosenberg 1991), being used as a distancing and re-framing technique in challenging situations and for fostering socialisation and group cohesion (Charman 2013). Its role in the development of student paramedics is also significant (Dean and Major 2008; Rosenberg 1991).
- Recommendations for future research and practice as a result of this review include:
- Investigating the effect of increases in female clinical staff numbers on the humour culture and staff resilience levels within the Ambulance Service.
- Examining the impact of initiatives such as ‘Make Ready’ and reduced time at base stations upon paramedic’s resilience to burnout.
- Exploring the socialisation process of student and newly registered paramedics into the Ambulance Service; the role humour plays in this and its effect on the development of group culture.
Chris Storey Paramedic Practice BSc (Hons) student
References
Alexander, D.A. and S. Klein. 2001. Ambulance personnel and critical incidents: impact of accident and emergency work on mental health and emotional well-being. British Journal of Psychiatry 178(1)76-81.
Babbie, E.R. 2009. The practice of social research. 12th ed. Belmont: Wadsworth Publishing.
Baid, H. and N. Lambert. 2010. Enjoyable learning: the role of humour, games and fun activities in nursing and midwifery education. Nurse Education Today 30(6) 548-552.
Beck, C. T. 1997. Humor in nursing practice: A phenomenological study. International Journal of Nursing Studies 34(5) 346-352.
Bennett, H.J. 2003. Humour in medicine. Southern Medical Journal 96(12) 1257-1261.
Bennett, P., Y. Williams., N. Page., K. Hood. and M. Woollard. 2004. Levels of mental health problems among UK emergency ambulance workers. Emergency Medical Journal 21(2) 235-236.
Bishop, A. 2013. Question regarding patient information. [email] Personal email to C. Storey. [11 November 2013].
Blau, G. and S. Chapman. 2011. Retrospectively exploring the importance of items in the decision to leave the emergency medical services (EMS) profession and their relationships to life satisfaction after leaving EMS and likelihood of returning to EMS. Journal of Allied Health 40(2) 29-32.
Burns, N. and S.K. Grove. 2001. The practice of nursing research: conduct, critique and utilization. 4th ed. Philadelphia: W.B. Saunders.
Buxman, K. 2008. Humor in the OR: a stitch in time? Association of Peri-Operative Registered Nurses Journal 88(1) 67-77.
Charman, S. 2013. Have you heard the one about the emergency services’ joke-book? Ambulance Today 2013 (Autumn) 41-43.
Chase, R. 2014. Stress and burnout. [Online]. Available at: http://www.emsvillage.com/articles/article.cfm?id=1044 (Accessed 29/1/14).
Chinery, W. 2007. Alleviating stress with humour: a literature review. [Online] Available at: http://www.redorbit.com/news/health/920164/alleviating_stress_with_humour_a_literature_review/ (Accessed 1/3/14).
Collins English Dictionary. 2011. 11th ed. Glasgow: Harper-Collins.
Cousins, N. 1979. Anatomy of an illness: as perceived by the patient: reflections on healing and regeneration. PDF [Online]. Available at : http://playpen.meraka.csir.co.za/~acdc/education/Dr_Anvind_Gupa/Learners_Library_7_March_2007/Resources/books/Anatomy.PDF (Accessed 1/3/14).
Data Protection Act. 1998. London: Stationary Office.
Dean, R.A.K. and J.E. Major. 2008. From critical care to comfort care: the sustaining value of humour. Journal of Clinical Nursing 17(8) 1088-1095.
Department of Health. 2003. Confidentiality – NHS code of practice. Norwich: Stationery Office.
Department of Health. 2009. NHS health and well-being: final report. [Boorman Review]. Norwich: Stationery Office.
Downe, P.J. 1999. Laughing when it hurts: humour and violence in the lives of Costa Rican prostitutes. Women’s Studies International Forum 22(1) 63-78.
Dyck, K.T.H. and S. Holtzman. 2013. Understanding humor styles and well-being: the importance of social relationships and gender. Personality and Individual Differences 2013 55(1) 53-58.
Dyrbye, L.N., D.V. Power., F.S. Massie., A. Eacker., W. Harper., M.R. Thomas., D.W. Szydlo., J.A. Sloan. and T.D. Shanafelt. 2010. Factors associated with resilience to and recovery from burnout: a prospective, multi-institutional study of US medical students. Medical Education 44(10) 1016-1026.
Essex, B. and L. Benz-Scott. 2008. Chronic stress and associated coping strategies among volunteer EMS personnel. Prehospital Emergency Care 12(1) 69-75.
Fabry, D. 2011. Hello to humour and goodbye to burnout. Audiology Today March/April 2011 36-37.
Feagai, H.E. 2011. Let humour lead your nursing practice. Nurse Leader August 2011 44-46.
Felton, J.S. 1998. Burnout as a clinical entity – its importance in healthcare workers. Occupational Medicine 48(4) 237-250.
Frank, J.R. and H. Ovens. 2002. Shift work and emergency medical practice. Canadian Journal of Emergency Medical Care 4(6) 421-428.
Freud, S. 2002. The joke and its relation to the unconscious: translated by J. Crick. London: Penguin.
Gayton, S.D. and G.P. Lovell. 2012. Resilience in ambulance service paramedics and its relationship with well-being and general health. Traumatology 18(1) 58-64.
Giddens, A. and P.W. Sutton. 2013. Sociology. 7th ed. Cambridge: Polity Press.
Glasberg, A.L., S. Eriksson. and A. Norberg. 2007. Burnout and ‘stress of conscience’ among healthcare personnel. Journal of Advanced Nursing 54(4) 392-403.
Goffman, E. 1959. The presentation of self in everyday life. New York: Doubleday.
Gonzalez-Roma, V., W. B. Schaufeli., A.B. Bakker. and S. Lloret. 2006. Burnout and work engagement: independent factors or opposite poles? Journal of Vocational Behaviour 68(1) 165-174.
Grafton, E., B. Gillespie. and S. Henderson. 2010. Resilience: the power within. Oncology Nursing Forum 37(6) 698-705.
Griner, P.F. 2013. Burnout in healthcare providers. Journal of Integrative Medicine 12(1) 22-24.
Gustafsson, G., S. Eriksson., G. Strandberg. and A. Nordberg. 2010. Burnout and perceptions of conscience among healthcare personnel: a pilot study. Nursing Ethics 17(1) 23-38.
Halpern, J., R.G. Maunder., B. Swartz. and M. Gurevich. 2012. Identifying, describing and expressing emotions after critical incidents in paramedics. Journal of Traumatic Stress 25(1) 111-114.
Harrington, J.M 2001. Health effects of shift work and extended hours of work. Occupational and Environmental Medicine 58(1) 68-72.
Hart, C. 2005. Doing a literature search: a comprehensive guide for the social sciences. London: Sage.
Hawkins, D. A. 2008. Comparing the use of humor to other coping mechanisms in relation to Maslach’s theory of burnout. PhD dissertation. University of Florida. [Online]. Available via online library at: http://gradworks.umi.com/33/22/3322923.html (Accessed: 1/3/14).
Health and Care Professions Council. 2012. Standards of conduct, performance and ethics. London: HCPC.
Health and Care Professions Council. 2013. Registrants gender split: November 2013. Freedom of information log. [Online]. Available via online library at http://hcpc-uk.co.uk/publications/foi/ (Accessed 18/6/14).
Health and Safety at Work Act: 1974. Chapter 37. 1974. Norwich: Stationery Office.
Henman, L.D. 2001. Humour as a coping mechanism: lessons from P.O.Ws. Humour 14(1): 83-94. PDF. [Online]. Available via online library at: http://sophiemin.files.wordpress.com/2013/12/humr-14-1-83.pdf. (Accessed 1/3/14).
Kaschka, W.P., D. Korczak. and K. Broich. 2011. Burnout – a fashionable diagnosis. Deutsches Arzteblatt International 108(46) 781-787.
Kuiper, N.A. 2012. Humor and resiliency: towards a process model of coping and growth. Europe’s Journal of Psychology 8(3) 475-491.
Lobiondo-Wood, G. and J. Haber. 2002. Nursing research: methods, critical appraisal and utilization. St Louis: Mosby.
Macnee, C.L. and S. McCabe. 2008. Understanding nursing research: reading and using research in evidence-based practice. 2nd ed. Philadelphia: Lippincott Williams and Wilkins.
Mahony, D.L. 2000. Is laughter the best medicine or any medicine at all? Psi Chi: The International Honor Society in Psychology 4(3) [Online] Available via online library at: http://www.psichi.org/?page=043EyeSpring00bMahon&hhSearchTerms=%22is+and+laughter+and+best+and+medicine%22 (Accessed 3/3/14).
Mahony, K. 2003. The politics of professionalisation: some implications for the occupation of ambulance paramedics in Australia. The Australian Journal of Paramedicine 1(3) 1-8.
Maslach, C. and M.P. Leiter. 2005. Reversing burnout: How to rekindle your passion for work. Stanford Social Innovation Review. Winter 2005: 43-49. [Online] Available via online library at: http://wellmd.stanford.edu/documents/Reversing%20Burnout.pdf (Accessed 29/1/14).
McAlister, M. and J. McKinnon. 2009. The importance of teaching and learning resilience in the health disciplines: a critical review of the literature. Nurse Education Today 29(4) 371-379.
McCarroll, J.E., R.J. Ursano., K.M. Wright. and C.S. Fullerton. 1993. Handling bodies after violent death: strategies for coping. American Journal of Orthopsychiatry 63(2): 209-214. PDF [Online]. Available via online library at: http://onlinelibrary.wiley.com/doi/10.1037/h0079438 PDF. ADA264372. (Accessed 10/5/14).
McGhee, P. 2013. Humour and Nursing 2: Using humour to cope with the challenges of nursing. Online Continuing Education for Nurses: Corexel. PDF. [Online] Available at: http://www.corexcel.com/courses/Humor_and_Nursing_II_Course_Handout.pdf (Accessed 1/3/14).
Moran, C. 1990. Does the use of humor as a coping strategy affect stresses associated with emergency work? International Journal of Mass Emergencies and Disasters 8(3) 361-377.
Moran, C. and M. Massam. 1997. An evaluation of humour in emergency work. The Australian Journal of Disaster and Trauma Studies March 1997. [Online] Available via online library at: http://www.massey.ac.nz/~trauma/issues/1997-3/moran1.htm (Accessed: 1/3/14)
Moule, P. and M. Goodman. 2009. Nursing research: an introduction. London: Sage.
Munhall, P.L. 2007. Nursing Research: a qualitative perspective. 4th ed. London: Jones and Bartlett.
Murphy, S., R.D. Beaton., K.C. Pike. and K.C. Cain. 1994. Firefighters and paramedics: years of service, job aspirations, and burnout. American Association of Occupational Health Nurses Journal 42(11) 534-540.
N.H.S. Employers. 2012. Welcome to the Team: Ambulance Service Staff. N.H.S. Employers.
Nirel, N., R. Goldwag., Z. Feigenberg., D. Abadi. and P. Halpem. 2008. Prehospital Disaster Medicine 23(6) 537-546.
Obrdlik, A.J. 1942. ‘Gallows humour’. American Sociological Review 47(5): 709-713. [Online] Available via online library at: http://www.jstor.org/discover/10.2307/2769536?uid=3738032&uid=2129&uid=2134&uid=379017161&uid=2&uid=70&uid=3&uid=379017151&uid=60&sid=21103747881591. (1/3/2014).
Okougha, M. 2013. Promoting patient care through staff development. Nursing Standard. 27 (34) 42-46.
Olson, M.L., D.S. Hugelshofer., P. Kwon. and R.C. Reff. 2005. Rumination and dysphoria: the buffering role of adaptive forms of humor. Personality and Individual Differences 39(8) 1419-1428.
Parahoo, K. 2006. Nursing research: principles, process and issues. 2nd ed. Basingstoke: Palgrave Macmillan.
Polit, D.F. and C.T. Beck. 2004. Nursing research: principles and methods. 7th ed. Philadelphia: Lippincott Williams & Wilkins.
Polit, D.F. and C.T. Beck. 2006. Essentials of nursing research: methods, appraisal and utilization. 6th ed. Philadelphia: Lippincott Williams & Wilkins.
Polit, D.F. and C.T. Beck. 2010. Essentials of nursing research: appraising evidence for nursing practice. 7th ed. Philadelphia: Lippincott Williams & Wilkins.
Popa, F., A. Raed., V.L. Purcarea., A. Lala. and G. Bobimac. 2010. Occupational burnout levels in emergency medicine – a nationwide study and analysis. Journal of Medicine and Life 3(3) 207-215.
Regehr, C. 2005. Bringing home the trauma: spouses of paramedics. Journal of Loss and Trauma 10(2) 97-114.
Rosenberg, L. 1991. A qualitative investigation of the use of humor by emergency personnel as a strategy for coping with stress. Journal of Emergency Nursing 17(4) 197-203.
Rowe, A. and C. Regehr. 2010. Whatever gets you through today: an examination of cynical humor among emergency service professionals. Journal of Loss and Trauma 15(5) 449-464.
Ruysschaert, N. 2009. (Self) Hypnosis in the prevention of burnout and compassion fatigue for caregivers: theory and induction. Contemporary Hypnosis 26(3) 159-172.
S.E.C.Amb. 2013. Annual Report and Accounts: 1st April 2012 – 31st March 2013. Banstead: S.E.C.Amb.
Scott, T. 2007. Expressions of humour by emergency personnel involved in sudden deathwork. Mortality 12(4) 350-364.
Shakespeare-Finch, J. and S. Savill. 2013. An investigation into the lived experience of intensive care paramedics. Australia and New Zealand Disaster Emergency Conference: 28th-31st May 2013. [Online]. PDF. Available at: http://eprints.qut.edu.au/62197/1/S-FandSavill2013.pdf (Accessed: 19/5/14).
Shepherd, L. and J. Wild. 2014. Cognitive appraisals, objectivity and coping in ambulance workers: a pilot study. Emergency Medical Journal 31(1) 41-44.
Sofianopoulos, S., B. Williams. and F. Archer. 2012. Paramedics and the effects of shift work on sleep: a literature review. Emergency Medical Journal 29(2) 152-155.
Stassen, W., B.V. Nugteren. and C. Stein. 2013. Burnout among advanced life support paramedics in Johannesburg, South Africa. Emergency Medical Journal 30(4) 331-333.
Steiger, S., A.K. Formann. and C. Burger. 2011. Humor styles and their relationship to explicit and implicit self-esteem. Personality and Individual Differences 50(5) 747-750.
Sterud, T., E. Hem., B. Lau. and O. Ekeberg. 2008. Suicidal ideation and suicide attempts in a nationwide sample of operational Norwegian ambulance personnel. Journal of Occupational Health 50(5) 406-414.
Strumpfer, D. J.W. 2003. Resilience and burnout: A stitch that could save nine. South African Journal of Psychology 33(2) 69.
Thomas, D.R. 2003. A general inductive approach for qualitative data analysis. PDF. [Online]. Available via online library at: http://www.frankumstein.com/PDF/Psychology/Inductive%20Content%20Analysis.pdf. (Accessed 19/4/14).
Van der Ploeg, E. and R.J. Kleber. 2003. Acute and chronic job stressors among ambulance personnel: predictors of health symptoms. Occupational Environmental Medicine 60(supplement) 40-46.
Van Wormer, K. and M. Boes. 1997. Humour in the emergency room: a social work perspective. Health and Social Work 22(2) 87-92.
Weisenberg, M., I. Tepper. and J. Schwarzwald. 1995. Humor as a cognitive technique for increasing pain tolerance. Pain 63(2) 207-212.
Watson, K. 2011. ‘Gallows humor in medicine’. Hastings Center Report 41(5): 37-45. [Online]. Available via online library at: http://www.thehastingscenter.org/Publications/HCR/Detail.aspx?id=5505 (Accessed: 27/2/14).
Whitmore, D. 2013. A paramedic’s experience of the 7 / 7 bombings. [Lecture] Student Paramedic Conference 17th July 2013. Kingston & St Georges University. London.
Williams, A. 2012. Emotion work in paramedic practice: the implications for nurse educators. Nurse Education Today 12(32) 368-372.
Williams, A. 2013. The strategies used to deal with emotion work in student paramedic practice. Nurse Education in Practice 13(13) 207-212.
Williams, A. 2013. A study of emotion work in student paramedic practice. Nurse Education Today 13(33) 512-517.
 On behalf of the Centre for Health Research it is a pleasure to have been invited to write a small piece for the inaugural issue for our new journal. This is a very welcome development for the new School of Health Sciences and I would like to thank all the members of the editorial team for all their hard work and commitment in putting the first issue of this journal together. I wish the journal well for all its future developments. Writing about and reporting regularly on research and scholarly activities is an important component of all academic members of staff routine activity. Sometimes early on in your career this can be a challenging concept and your confidence may be lacking in terms of your ability to write and to publish in an academic journal. The Journal has been set up by the editors to nurture and support members of staff and students who wish to write for an academic journal. It is anticipated that the editors’ and reviewers’ comments on your work will help to strengthen your manuscript. Through this you will learn more about how to craft research and scholarly papers that sit within your field of practice.The Journal will also give all staff the opportunity to publish their research news and thereby share research activities across the school. The journal is therefore a very welcome development in this new school and I look forward to seeing this development over
On behalf of the Centre for Health Research it is a pleasure to have been invited to write a small piece for the inaugural issue for our new journal. This is a very welcome development for the new School of Health Sciences and I would like to thank all the members of the editorial team for all their hard work and commitment in putting the first issue of this journal together. I wish the journal well for all its future developments. Writing about and reporting regularly on research and scholarly activities is an important component of all academic members of staff routine activity. Sometimes early on in your career this can be a challenging concept and your confidence may be lacking in terms of your ability to write and to publish in an academic journal. The Journal has been set up by the editors to nurture and support members of staff and students who wish to write for an academic journal. It is anticipated that the editors’ and reviewers’ comments on your work will help to strengthen your manuscript. Through this you will learn more about how to craft research and scholarly papers that sit within your field of practice.The Journal will also give all staff the opportunity to publish their research news and thereby share research activities across the school. The journal is therefore a very welcome development in this new school and I look forward to seeing this development over